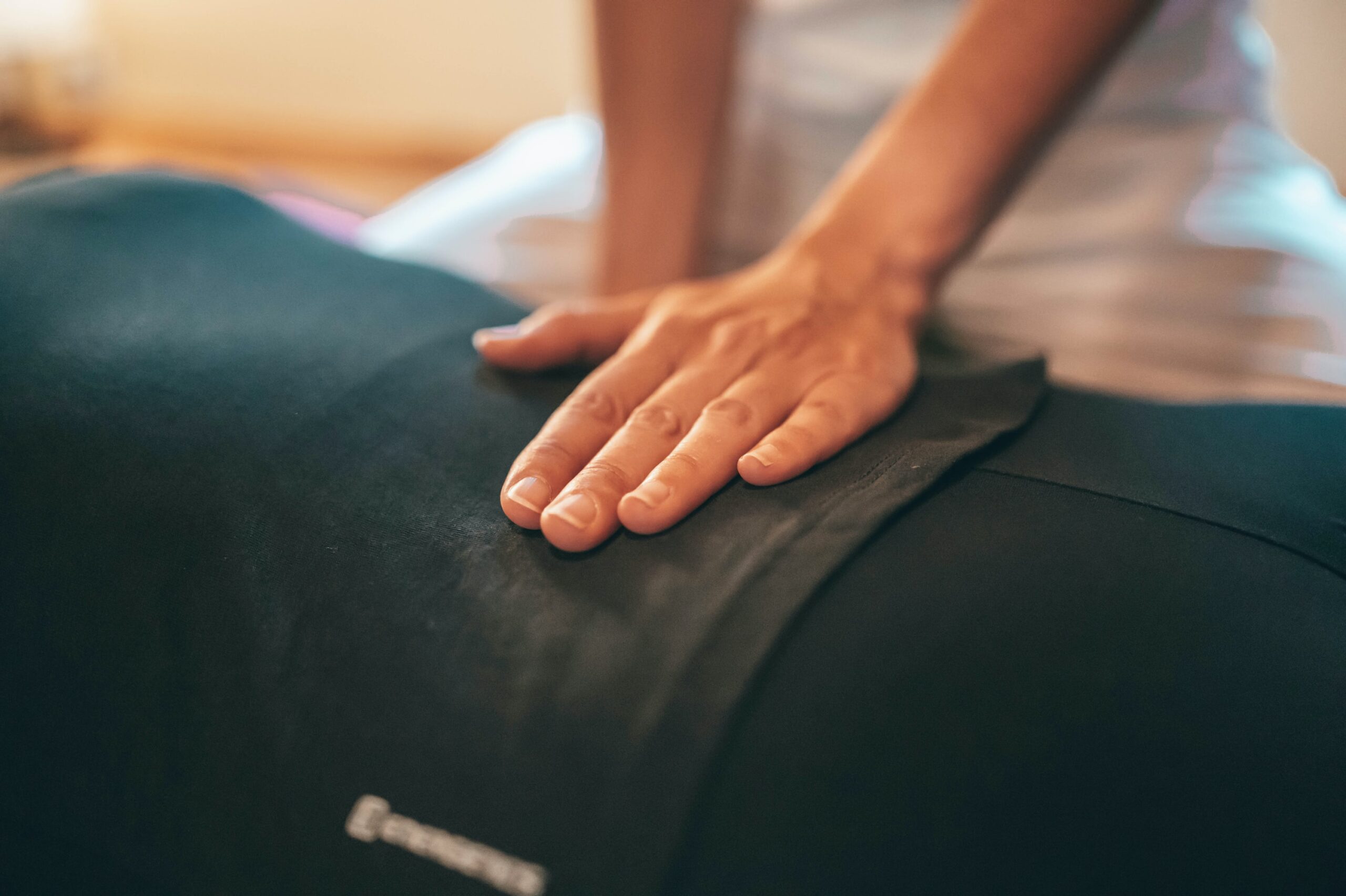
Physical Therapy Before Excision Surgery for Endometriosis
Endometriosis can cause multiple issues for our bodies and can create the need for a multidisciplinary care team to address chronic pelvic pain. Physical therapy is one example of part of a multidisciplinary treatment plan for endometriosis symptoms. Guest writer Rebecca Patton, PT, DPT, discusses considerations for using physical therapy while awaiting excision surgery:
Pelvic physical therapy has gained more following and prompted much needed discussions in recent years. However, pelvic physical therapy looks quite different for someone with chronic pelvic pain and endometriosis.
The reality is that pelvic physical therapists may be a first line of defense to refer a patient to a specialist. First, because we have direct access, meaning a patient can see us for an evaluation before seeing a physician. Second, because symptoms of endometriosis are often missed or dismissed by referring providers. In the latter case, someone may be referred to physical therapy before excision surgery or even before seeing an endo specialist.
Top endometriosis physical therapists
Endometriosis Physical Therapy
pelvic floor therapy for endometriosis
Physical therapists can optimize care by helping a patient get to a specialist while providing physical therapy treatment.
If we are seeking to provide the best care available for treatment of endo, getting faster diagnosis and referring a patient to an excision specialist is the primary goal. With a thorough medical history including bowel and bladder habits, menstrual symptoms, pelvic pain symptoms, previous treatment, and understanding the patient’s experience, a pelvic physical therapist can create a differential diagnosis list that may include endometriosis. If endometriosis is suspected, a referral to an excision specialist should be given to the patient and explained.
Endo specialists’ wait times vary greatly depending on where you are located.
In my personal experience in Phoenix, AZ, a large metropolitan area with several specialists, it takes anywhere from 3-12 months. More time if we are in the middle of a global pandemic. Decreased access in rural areas may also increase waiting times. One positive change is the inclusion of virtual appointments which may improve access for those in rural areas.
During the waiting period, the goal is to manage pain and maintain some regularity with bowel and bladder habits until excision surgery. Internal pelvic floor retraining may or may not be appropriate during this time.
As mentioned before, physical therapy before excision surgery is going to look different from treatments for other conditions. As a patient, you want to ensure the physical therapist you are seeing treats patients with endo regularly. You may want to consult with them prior about how often they treat patients with endo and what treatments they use specifically. Additional coursework for visceral and abdominal manual therapy techniques, nerve mobilization, and myofascial therapy techniques will be helpful.
Most studies research the effectiveness of physical therapy following excision surgery. What about physical therapy before excision surgery?
Zhao et al. (1) found that 12 weeks of PMR (progressive muscle relaxation) training is effective in improving anxiety, depression and QOL of endometriosis patients under GnRH agonist therapy. These participants had not received excision surgery.
Awad et al. (2) found improvements in posture and pain with an 8-week regular exercise program in those diagnosed with mild to moderate endometriosis. This exercise program included posture awareness, diaphragm breathing, muscle relaxation techniques, lower back and hip stretches, and walking. Of note, this exercise program was not vigorous exercise. These participants were also receiving hormonal treatment but not receiving pain medication.
Both studies did not say that physical exercise or PMR plays a role in the prevention of the occurrence or progression of endometriosis. Both studies were short term (8-12 weeks) and did not explore pain management directly before excision or outcomes after excision.
In the time that a patient is waiting for excision surgery, I believe physical therapy treatment can be effective at minimizing overall pain levels and improving quality of life.
A few factors to keep in mind if you are seeking pelvic physical therapy before excision surgery:
- Your symptoms after physical therapy should not last more than 1-2 days and should feel manageable. Being bedridden for a week after physical therapy is not a helpful treatment. If you experience this, be sure to communicate it with your physical therapist to adjust the plan. Not all pelvic PT’s are experienced with this type of treatment and they may create an exercise plan that is too vigorous.
- Internal pelvic floor treatment is not always the most helpful in this situation and may exacerbate symptoms. An individualized plan is important to discuss with your provider.
- You are in charge of your body. If you don’t feel like a treatment is working then communicate that to your team and discuss other options. It is always okay to voice your concerns to change the treatment to fit you best.
- Treatment before surgery requires a multidisciplinary team. This may include other pain management options including medication.
iCareBetter is doing the ground work to vet pelvic physical therapists.
Rebecca Patton PT, DPT (If you are seeking a pelvic PT, I accept consultations through my website for in person and telehealth appointments: https://www.pattonpelvichealth.com/)
For more resources on physical therapy for endometriosis see: https://icarebetter.com/physical-therapy-resources/
References
Zhao L, Wu H, Zhou X, et al.: Effects of progressive muscular relaxation training on anxiety, depression and quality of life of endometriosis patients under gonadotrophin-releasing hormone agonist therapy. Eur J Obstet Gynecol Reprod Biol, 2012, 162: 211–215. [PubMed] [Google Scholar]
Awad E, Ahmed HAH, Yousef A, Abbas R. Efficacy of exercise on pelvic pain and posture associated with endometriosis: within subject design. J Phys Ther Sci. 2017;29(12):2112-2115. doi:10.1589/jpts.29.2112 [NCBI]

Choosing the Right Mental Health Therapist
By Deanna Denman, PhD, Licensed Psychologist, Clinical Health Psychologist
Find the right therapist can be just as difficult as finding an endometriosis specialist. There are many different types of therapists providing many different types of therapy out there, and “fit” between you and your therapist is very important. I’ve included some helpful information and tips below to help you find a good therapist if you’d like some support along your Endo journey.
- Finding a therapist-
-Expect to check out several therapists via website. Most therapists offer a free consultation to see if you both think it’s a good fit. The “fit” with you and your therapist is going to be important for your trust and ultimately your progress in therapy.
-If you meet with someone and they aren’t a good fit, that’s okay! You can even ask them if they have referrals for you.
-Ask your doctor if they have any recommendations. Some doctors have therapists they have worked with in the past and who they trust. Ask if your doctor has any referrals for you.
-There are SEVERAL therapist directories. Search them for therapists in your area. I encourage you to check out:
- Inclusive Therapists
- Psychology Today
- Therapy for Black Girls
- Therapy for Latinx
- QTPOC
- Your insurance company (they usually list covered providers on their website)
- Your network (friends, family, co-workers) if you are comfortable
**Some people prefer to work with therapists who hold similar identities to them. I’ve included some resources for therapists of color and LGBTQ+ therapists in the list above***
2. What to ask-
So you’ve found a few potential therapists. What should you ask in the first consultation:
-How much do sessions cost?
Therapy is an investment in your well-being, but I know costs can be prohibitive! BE thoughtful and open about your budget for therapy. Many therapists list their rates online as well as whether or not they accept insurance. Some therapists don’t accept insurance, but will still provide you with a receipt for services that you can provide to your insurance for reimbursement. ***Talk to your insurance provider about your out-of-network mental health benefits.***
-How much experience and what trainings do you have in working with people with endometriosis?
(You can also ask about other things you’d like to work on in therapy like trauma, anxiety, or even people-pleasing). Really anything is fair game, but it’s important to assess their comfort level with your particular concerns. Specifically, if you are seeking support with your Endo, you want to know if they are familiar with the condition, if they are comfortable in collaborating with your medical providers, and what kinds of interventions they use. If they have never worked with someone with chronic pain, or their only recommendation for someone with chronic pain is to start exercising, they’re not likely to be a good fit.
–How will we set goals/measure progress?
Ideally, you want to set goals together with your therapist. You should also check in regularly about how you are doing and the plan for moving forward
3. Credentials-
If you’ve ever been confused by the alphabet soup after therapists’ names, you’re not alone. The conversation around the differences between “counseling” and “therapy” are beyond the scope of this post. Most people use the terms interchangeably and the right provider for you could fall into either category.
***Note: any provider you work with must be licensed to practice (or pursuing licensure and working under supervision)***
Let’s break it down:
Professional Counselors
- LPC- licensed professional counselor (may have -A, -S behind LPC to designate “associate” or “supervisor”)
- LMHC- licensed mental health counselor
- LCADAC- licensed clinical alcohol and drug abuse counselor
- LMFT- licensed marriage and family therapist
Broadly, counselors are more focused on helping you solve mental health and behavioral problems and giving you very practical skills.
*LMFTs are not technically counselors (their title even includes ‘therapist’), but they best fit in this category, and tend to specialize in things influenced by relationships. LMFTs DO offer individual therapy and often have specialty training in concerns like infertility.
Social Workers
- LCSW- licensed clinical social worker (may have -A, or -C behind LCSW to designate “associate” or “certified”)
- LISW- licensed independent social worker
- MSW- Master of social work (the degree)
Again, broadly, social workers are very well trained to address social and environmental issues (think: systems of oppression and “isms”) and problem-solve. They also tend to be very knowledgeable about resources (like programs and trainings) that can help you.
Psychologists
- PhD- doctor of philosophy
- PsyD- doctor of psychology
Generally, psychologists focus on very complex issues and very strongly grounded in theories of mental health. They tend to be more assessment-, and research-, focused due to their training. (They can also do psychological testing for things like memory and learning disabilities)
These are all very broad generalizations and still don’t address people’s specialties (the populations they focus on), the theory they are grounded in, or the interventions they use. The best place to get a sense of that is by reading their websites and speaking with them directly.
What’s important- regardless of the letters, most of them are trained to help people work things out in therapy. They will NOT all have the training to help with issues around endometriosis. That’s why taking advantage of the consultation is important.
4. Specialties-
Therapists often have specialties. Realistically, you can find therapists specializing in just about anything. There are some therapists who specialize in trauma, others who specialize in working with high-achievers who want to slow down. There are ALSO therapists who specialize in working with patients who have chronic illness. You may want to see a provider who has specialty training and focus in working with patients with chronic illness. Finding the right therapist for you can take some effort but is worth it. Consider what you’d like to address and look for therapists who speak to that on their sites/listings. If you can, take advantage of free consultations. Ask potential therapists about their experience and training in your concerns. Be open to trying more than one and know that personality fit is important. It’s okay to search until you find the right support for you on this endometriosis journey.

Endo diet: Mediterranean or FODMAP for the win?
A healthy eating pattern can be therapeutic and good for our health overall, but it can be difficult to decide on what is best for our bodies. The process can involve a long time spent in trial and error to find what works for our individual body and its needs. When looking at studies on dietary interventions, we find that they are difficult to perform- often ending up with strong bias or high inconsistent rates with adherence (anyone else here ever cheat on a diet??). But they can give us some direction. For instance, a systematic analysis by Nirgianakis et al. (2021) looked at a few recent studies on diet’s effect on endometriosis symptoms. While, unfortunately, the data was not strong enough for any strong conclusions, it can give some clues for individuals with endometriosis (along with consultation with a healthcare provider).
Two of the diets looked at included the Mediterranean diet and a diet low in fermentable oligo-, di-, monosaccharides, and polyols (FODMAP). Both showed promise for help with endometriosis symptoms, particularly gastrointestinal symptoms and pain.
Nirgianakis et al., (2021) explains:
“FODMAPs are poorly absorbed, short-chain carbohydrates that are readily fermentable by bacteria. Their osmotic actions and gas production may cause intestinal luminal distension inducing pain and bloating in patients with visceral hypersensitivity with secondary effects on gut motility….Diseases like irritable bowel syndrome and endometriosis come along with visceral hypersensitivity, implementing the hypothesis of symptom-reduction after sticking to a low-FODMAP diet. This is very important given the high prevalence of gastrointestinal-related symptoms and co-morbidities in patients with endometriosis. Interestingly, the low-FODMAP diet includes not only a low-Ni diet, but also a low-lactose and a low-gluten diet, thus covering the above-mentioned diets and a large spectrum of high-prevalence pathologies, such as lactose intolerance and non-celiac gluten sensitivity. It is therefore possible to obtain clinical benefits from a low-FODMAP diet, even if at the cost of probably not necessary dietary exclusions.”
The Mediterranean diet includes “fresh vegetables, fruit, white meat, fish rich in fat, soy products, whole meal products, foods rich in magnesium, and cold-pressed oils,” while avoiding “sugary drinks, red meat, sweets, and animal fats”. The review noted that “a significant relief of general pain, dysmenorrhea, dyspareunia, and dyschezia as well as an improvement in the general condition was found.” Moreover, the “Mediterranean diet has well-known antioxidant effects. However, the Mediterranean diet does not involve just the supplementation of certain antioxidants, but rather a collection of eating habits and may thus improve endometriosis-associated pain via additional mechanisms. Fish as well as extra virgin olive oils have been shown to exert anti-inflammatory effects. Specifically, extra virgin olive oil, which contains the substance oleocanthal, displays a similar structure to the molecule ibuprofen, and both take effect via the same mechanism, i.e., cyclooxygenase inhibition. Moreover, the increased amount of fibers provides a eupeptic effect while foods high in magnesium could prevent an increase in the intracellular calcium level and advance the relaxation of the uterus. Taking into account the lack of risks or side effects even after long-term lifetime adherence to this diet and the possible other general health benefits, clinicians may suggest this type of dietary intervention to patients with endometriosis who wish to change their nutritional habits.”
Finally, the authors looked at a qualitative study and found that “the participants experienced an increase in well-being and a decrease in symptoms following their dietary and lifestyle changes. They also felt that the dietary changes led to increased energy levels and a deeper understanding of how they could affect their health by listening to their body’s reactions.” So, taking control of your diet can help improve your general sense of well-being.
Again, there was not strong evidence from any of the studies reviewed, but it might prove helpful when discussing complementary therapies with your healthcare provider. You can find more information about diet and endometriosis here.
Reference
Nirgianakis, K., Egger, K., Kalaitzopoulos, D. R., Lanz, S., Bally, L., & Mueller, M. D. (2021). Effectiveness of Dietary Interventions in the Treatment of Endometriosis: a Systematic Review. Reproductive Sciences, 1-17. Retrieved from https://link.springer.com/article/10.1007/s43032-020-00418-w

Life altering disease and caregivers
Endometriosis can have a profound effect on a person’s ability to work, care for their home, care for their family, and even care for themselves- and this impacts their loved ones as well (Missmer et al., 2021). Endometriosis can have a “negative impact on intimate relationships” (Facchin et al., 2021). It is essential for the person with endometriosis and their support person(s) to have a plan to take care of both of themselves.
The impact endometriosis has on the activities of daily life is not well understood by the general population. This makes it difficult for even loved ones and family members to understand why you may be so fatigued or in too much pain some days to do what you might be able to other days- not to mention the emotional toll it can have. Education for loved ones about the disease itself is important as is education about the treatment. To “minimize the negative impact of endometriosis” on an individual’s life course, “early diagnosis and effective intervention in treating the disease” is imperative (Missmer et al., 2021). This is what we advocate for so strongly- early diagnosis and effective treatment to minimize the impact on a person’s life!
Once your support person or caregiver has a better understanding of the disease and its treatment, you can both develop a plan on how to handle its impact on your lives. Endometriosis can be life altering for those of us with it and those around us. It is important to address the way endometriosis affects our daily lives and have a plan to care for ourselves and our caregivers. This could be parents, partners, children, and various other loved ones involved in our lives. Each might have a different role to play and its good to have a collective plan to lessen the detrimental effects of endometriosis.
For those of us with endometriosis, remember it’s okay to need help. It is easy to feel guilty about not being able to do things, but don’t feel guilty for the effects of a chronic illness. You are doing the best you can. Accept help when it’s offered. Be realistic about what you need to live your best life possible where you are at. Borrowing from the Marine Corps, we have to improvise and adapt if we are to overcome. You are worth the effort.
For the caregivers in our lives- thank you. You’ll never know how much it means to have someone love, understand, and support us on this difficult journey. There are many of us who don’t have that support in our lives and are most acutely aware of how much it would mean. We want you to take care of yourself too. The following is for anyone who is in a caregiver role (including those of us with endometriosis who are in a caregiver role as well):
Being a support person or a caregiver can be both difficult and rewarding. When you start to feel the weight of it, there is a nursing diagnosis for it called “caregiver role strain” (Wayne, 2017). “While caregiving can be rewarding and positive, many family caregivers experience significant physical, psychological, and financial stressors in association with their caregiving role” (Wayne, 2017). This strain can come from multiple factors, such as unrealistic expectations (you won’t be able to fix us), juggling multiple roles (such as income earner, caregiver to other family members), lack of a support system (especially with a disease that others may not understand or may even trivialize), financial pressures, demands of care, social isolation, and neglecting your own well-being (FreedomCare, 2020).
From Wayne (2017), here are some things that might help with reducing caregiver role strain:
- Set aside time for yourself. Take care of your own physical and emotional needs. You can’t pour from an empty cup- you need time to rebuild your physical and emotional energy.
- Utilize stress-reducing methods- “It is important that the caregiver has the opportunity to relax and reenergize emotionally throughout the day to assume care responsibilities.”
- Participate in a support group if there is one available close by or online.
- Discuss problems, concerns, and feelings with a support person or a counselor. Sometimes you need someone outside the family to talk to. Taking on the caregiver role can change dynamics of the relationship and it can take effort to keep the “normal” relationship stuff going.
- Accept help! Ask and allow other available family and friends to assist with caregiving. “Successful caregiving should not be the sole responsibility of one person.”
- Make life chores easy on the both of you. For example, having occasional (or regular if you are able!) housekeeping services or deciding to get takeout food rather than cook one night can help relieve the burden sometimes. It’s okay if it’s not perfect.
Resources:
- Find more at: https://icarebetter.com/learning-library/patient-stories/
- Wondering if you are suffering from caregiver role strain? You can use the Modified Caregiver Strain Index to assess and talk to your healthcare provider about ways to help cope: https://www.sralab.org/sites/default/files/2017-07/issue-14.pdf
- Endowhat: “Caregivers” https://www.endowhat.org/caregivers
References
Facchin, F., Buggio, L., Vercellini, P., Frassineti, A., Beltrami, S., & Saita, E. (2021). Quality of intimate relationships, dyadic coping, and psychological health in women with endometriosis: Results from an online survey. Journal of Psychosomatic Research, 146, 110502. Retrieved from https://doi.org/10.1016/j.jpsychores.2021.110502
FreedomCare. (2020). What is caregiver strain and how to avoid it. Retrieved from https://www.freedomcareny.com/posts/caregiver-role-strain
Missmer, S. A., Tu, F. F., Agarwal, S. K., Chapron, C., Soliman, A. M., Chiuve, S., … & As-Sanie, S. (2021). Impact of endometriosis on life-course potential: a narrative review. International Journal of General Medicine, 14, 9. doi: 10.2147/IJGM.S261139
Wayne, G. (2017). Caregiver role strain nursing care plan. Retrieved from https://nurseslabs.com/caregiver-role-strain/
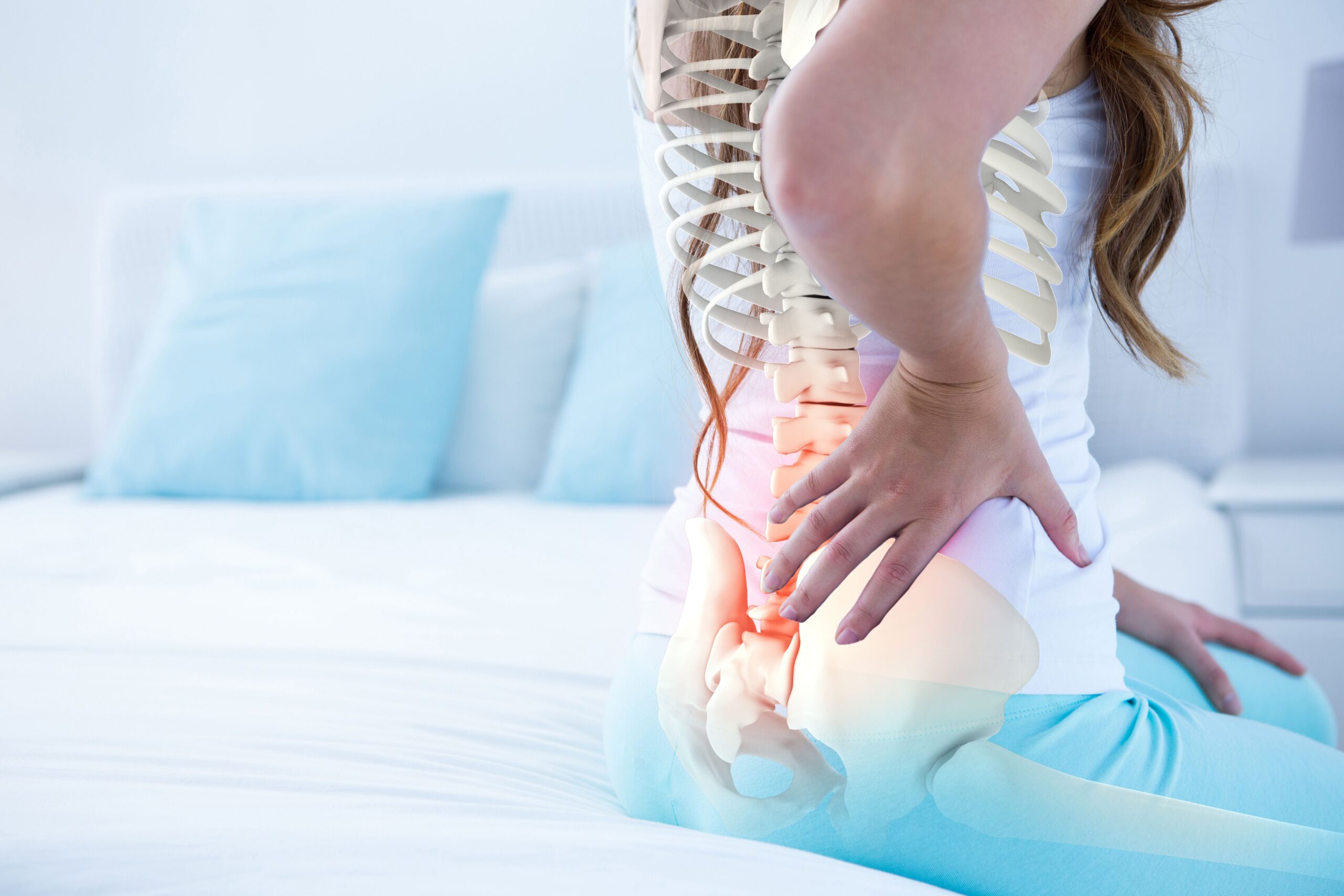
Insomnia and poor sleep with endometriosis
Sleep quality in individuals with endometriosis is significantly worse than those without it (Nunes et al., 2015). It seems like a no-brainer that pain and other symptoms from endometriosis can affect sleep quality. In fact, pain from endometriosis is known to affect a person’s “work/school, daily activities, exercise, and sleep to a moderate-extreme degree” (DiVasta et al., 2018). And in a vicious cycle, pain affects sleep and poor sleep affects pain. We get how pain can affect sleep, but what are the mechanics behind poor sleep affecting pain?
Ishikura et al. (2020) explains:
“It is well known that any pain condition can affect sleep, leading to sleep disturbances and impairment in sleep quality. In turn, sleep disruption can activate inflammatory mechanisms by triggering changes in the effector systems that regulate the immune system, resulting in abnormal increases in inflammatory responses that can stimulate or increase pain. This can result in the creation of a vicious cycle, with pain causing sleep disturbance that increases inflammation, leading to increased pain. Moreover, experimental studies have shown that the association of sleep loss and inflammatory markers are stronger in females than males, suggesting that women with both insomnia and endometriosis complaints are more susceptible to symptoms of pain. Endometriosis induces several debilitating symptoms that affect women´s lives, including insomnia; however, there have been very few studies of this association…. Treating insomnia would reduce the negative outcomes related to the inflammatory- and pain-related aspects of endometriosis and would contribute to an improvement in mental health and daytime function.”
This poor sleep can increase fatigue, affect quality of life, increase stress, and be detrimental to mental health in those with endometriosis (Arion et al., 2020; Ramin-Wright et al., 2018). Hormonal fluctuations within the menstrual cycle can affect sleep quality as well (drop in progesterone before menses, rise in body temperature during the luteal phase). Some hormonal treatments can affect sleep (Brown et al., 2008).
What can we do to help our sleep? Step one is to have a plan to address the underlying factors affecting sleep such as removing endometriosis. In the meantime, practice pain reduction techniques (nutrition,complimentary therapies such as yoga, pelvic physical therapy, etc.), practice good sleep hygiene, and talk to your healthcare provider about ways to manage pain and insomnia. One study indicated that “melatonin improved sleep quality” and “reduced the risk of using an analgesic by 80%” in patients with endometriosis (Schwertner et al., 2013). The American Academy of Sleep Medicine (2020) reports that cognitive behavioral therapy is the most effective therapy for chronic insomnia. They also suggest:
Keep a consistent sleep schedule. Get up at the same time every day, even on weekends or during vacations.
Set a bedtime that is early enough for you to get at least 7-8 hours of sleep.
Don’t go to bed unless you are sleepy.
If you don’t fall asleep after 20 minutes, get out of bed. Go do a quiet activity without a lot of light exposure. It is especially important to not get on electronics.
Establish a relaxing bedtime routine.
Use your bed only for sleep and sex.
Make your bedroom quiet and relaxing. Keep the room at a comfortable, cool temperature.
Limit exposure to bright light in the evenings.
Turn off electronic devices at least 30 minutes before bedtime.
Don’t eat a large meal before bedtime. If you are hungry at night, eat a light, healthy snack.
Exercise regularly and maintain a healthy diet.
Avoid consuming caffeine in the afternoon or evening.
Avoid consuming alcohol before bedtime.
Reduce your fluid intake before bedtime.
American Academy of Sleep Medicine (2020)
References
American Academy of Sleep Medicine. (2020). Healthy sleep habits. Retrieved from https://sleepeducation.org/healthy-sleep/healthy-sleep-habits/
Arion, K., Orr, N. L., Noga, H., Allaire, C., Williams, C., Bedaiwy, M. A., & Yong, P. J. (2020). A quantitative analysis of sleep quality in women with endometriosis. Journal of Women’s Health, 29(9), 1209-1215. Retrieved from https://www.liebertpub.com/doi/abs/10.1089/jwh.2019.8008
Brown, S. G., Morrison, L. A., Larkspur, L. M., Marsh, A. L., & Nicolaisen, N. (2008). Well-being, sleep, exercise patterns, and the menstrual cycle: a comparison of natural hormones, oral contraceptives and depo-provera. Women & health, 47(1), 105-121. Retrieved from https://doi.org/10.1300/J013v47n01_06
DiVasta, A. D., Vitonis, A. F., Laufer, M. R., & Missmer, S. A. (2018). Spectrum of symptoms in women diagnosed with endometriosis during adolescence vs adulthood. American journal of obstetrics and gynecology, 218(3), 324-e1. Retrieved from https://doi.org/10.1016/j.ajog.2017.12.007
Ishikura, I. A., Hachul, H., Pires, G. N., Tufik, S., & Andersen, M. L. (2020). The relationship between insomnia and endometriosis. Journal of Clinical Sleep Medicine, 16(8), 1387-1388. Retrieved from https://doi.org/10.5664/jcsm.8464
Nunes, F. R., Ferreira, J. M., & Bahamondes, L. (2015). Pain threshold and sleep quality in women with endometriosis. European Journal of Pain, 19(1), 15-20. Retrieved from https://doi.org/10.1002/ejp.514
Ramin-Wright, A., Schwartz, A. S. K., Geraedts, K., Rauchfuss, M., Wölfler, M. M., Haeberlin, F., … & Leeners, B. (2018). Fatigue–a symptom in endometriosis. Human reproduction, 33(8), 1459-1465. Retrieved from https://doi.org/10.1093/humrep/dey115
Schwertner, A., Dos Santos, C. C. C., Costa, G. D., Deitos, A., de Souza, A., de Souza, I. C. C., … & Caumo, W. (2013). Efficacy of melatonin in the treatment of endometriosis: a phase II, randomized, double-blind, placebo-controlled trial. PAIN®, 154(6), 874-881. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S030439591300081X

What’s all the buzz about the bowel?
The bloating, cramping, diarrhea, constipation, pain with bowel movements, nausea…could this be endometriosis?
Yes, it could.
Irritable bowel syndrome (IBS) like symptoms are common with endometriosis- up to 85% of endometriosis patients have gastrointestinal/bowel symptoms (Aragon & Lessey, 2017; Ek et al., 2015). It can be difficult to distinguish if it is endometriosis causing the IBS-like symptoms or if IBS is occurring along with endometriosis. Ek (2019) noted that “several potential shared pathophysiological mechanisms exist between endometriosis and IBS, such as chronic low-grade inflammation, increased mast cell numbers, increased mast cell activation, visceral hypersensitivity, altered gut microbiota and increased intestinal permeability, which has been described in relation to both endometriosis and IBS.” IBS symptoms can be helped with a low FODMAPs diet, and studies have noted that those with both IBS type symptoms AND endometriosis found improvement with a low FODMAPs diet (Moore et al., 2017). (See more info on bowel/GI endometriosis)
Endometriosis does not have to be on the bowel to cause bowel symptoms. Most of the time, symptoms may be due to irritation from lesions near the bowel (such as posterior cul de sac, Pouch of Douglas, uterosacral ligaments, etc.) or from adhesions pulling on the bowel (Aragon & Lessey, 2017; Ek et al., 2015). The incidence of endometriosis on the bowel itself ranges from 5% to 12% of those with endometriosis (Habib et al., 2020).
When endometriosis does involve the bowel, it most often found on the sigmoid colon, “followed by the rectum, ileum, appendix, and caecum” (Charatsi et al., 2018). “Extremely rare locations that have been reported include the gallbladder, the Meckel diverticulum, stomach, and endometriotic cysts of the pancreas and liver” (Charatsi et al., 2018). It can be difficult to determine bowel involvement from symptoms alone. Symptoms can range from none to crampy abdominal pain, constipation, diarrhea, pain with bowel movements, nausea, vomiting, and rarely rectal bleeding (Charatsi et al., 2018). Symptoms may be acyclical (all month long) and then aggravated during your period (Charatsi et al., 2018).
If your surgeon is suspicious of bowel involvement, they may do imaging prior to surgery to help guide care. Transvaginal ultrasounds and magnetic resonance imaging (MRIs) can be useful in detecting bowel involvement (but don’t necessarily rule it out) (Guerriero et al., 2018). According to one center that specializes in endometriosis surgery, “lesions on the colon, especially the distal sigmoid and rectum, I find ultrasound to be the most reliable” with the limitation that “it will only image the distal 20 cm of the colon, and lesions above that will be missed” (Pacific Endometriosis and Pelvic Surgery, n.d.). “For higher lesions on the sigmoid, the right colon, and small bowel then MRI is more accurate” (Pacific Endometriosis and Pelvic Surgery, n.d.).
Will surgery fix those IBS-like symptoms? It can be difficult to find studies that prove that. Mostly because “surgical techniques are not standardized” (Wolthuis et al., 2014). However, one center that specializes in endometriosis surgery found (with questionnaires of their patients) that their patients saw an “80% reduction in most bowel symptoms” (Center for Endometriosis Care, 2020). This rate may not be found with general gynecology surgery. If you think you might have bowel involvement, it is important to find the right care. The success of surgery depends on the skills and experience of the surgeon and a multidisciplinary team. It is recommended that “surgery should be performed by experienced surgeons, in centres with access to multidisciplinary care” (Habib et al., 2020, para. 1). While hormonal medications have been shown to help relieve symptoms, it may not stop the progression of the disease which can lead, in severe cases, to bowel obstruction; therefore, it is recommended that close follow-up be utilized if you do not choose surgical treatment (Habib et al., 2020; Ferrero et al., 2011).
- Interested in more info on bowel endo care from the experts? See the Endo Summit’s videos found on YouTube: https://www.youtube.com/watch?v=QJRkk4-6cSk and https://www.youtube.com/watch?v=BXUllhdW2h0
- For more on surgical technique for bowel endometriosis look here.
- You can search for surgeons with skill on bowel endometriosis here.
- Problems with pelvic floor dysfunction and other issues can also contribute to some symptoms- see Pelvic Floor Dysfunction
References
Aragon, M., & Lessey, B. A. (2017). Irritable Bowel Syndrome and Endometriosis: Twins in Disguise. GHS Proc, 43-50. Retrieved from https://hsc.ghs.org/wp-content/uploads/2016/11/GHS-Proc-Ibs-And-Endometriosis.pdf
Center for Endometriosis Care. (2020). Bowel endometriosis. Retrieved from https://centerforendo.com/endometriosis-and-bowel-symptoms
Charatsi, D., Koukoura, O., Ntavela, I. G., Chintziou, F., Gkorila, G., Tsagkoulis, M., … & Daponte, A. (2018). Gastrointestinal and urinary tract endometriosis: a review on the commonest locations of extrapelvic endometriosis. Advances in medicine, 2018. Retrieved from https://doi.org/10.1155/2018/3461209
Ek, M. (2019). Gastrointestinal symptoms in women with endometriosis. Aspects of comorbidity, autoimmunity and inflammatory mechanisms (Doctoral dissertation, Lund University).
Ek, M., Roth, B., Ekström, P., Valentin, L., Bengtsson, M., & Ohlsson, B. (2015). Gastrointestinal symptoms among endometriosis patients—A case-cohort study. BMC women’s health, 15(1), 59. doi: 10.1186/s12905-015-0213-2
Ferrero, S., Camerini, G., Maggiore, U. L. R., Venturini, P. L., Biscaldi, E., & Remorgida, V. (2011). Bowel endometriosis: Recent insights and unsolved problems. World journal of gastrointestinal surgery, 3(3), 31. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3069336/
Guerriero, S., Saba, L., Pascual, M. A., Ajossa, S., Rodriguez, I., Mais, V., & Alcazar, J. L. (2018). Transvaginal ultrasound vs magnetic resonance imaging for diagnosing deep infiltrating endometriosis: systematic review and meta‐analysis. Ultrasound in Obstetrics & Gynecology, 51(5), 586-595. Retrieved from https://obgyn.onlinelibrary.wiley.com/doi/full/10.1002/uog.18961
Habib, N., Centini, G., Lazzeri, L., Amoruso, N., El Khoury, L., Zupi, E., & Afors, K. (2020). Bowel Endometriosis: Current Perspectives on Diagnosis and Treatment. International Journal of Women’s Health, 12, 35. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6996110/
Moore, J. S., Gibson, P. R., Perry, R. E., & Burgell, R. E. (2017). Endometriosis in patients with irritable bowel syndrome: specific symptomatic and demographic profile, and response to the low FODMAP diet. Australian and New Zealand Journal of Obstetrics and Gynaecology, 57(2), 201-205. Retrieved from https://doi.org/10.1111/ajo.12594
Pacific Endometriosis and Pelvic Surgery. (n.d.) Bowel disease. Retrieved from https://pacificendometriosis.com/bowel-disease/?fbclid=IwAR1EVUZJHHVk7wvdGwTwJ6Mo8QICiY8ktRtCXIotvhQzKqvTqa0LSjEZs-k
Wolthuis, A. M., Meuleman, C., Tomassetti, C., D’Hooghe, T., van Overstraeten, A. D. B., & D’Hoore, A. (2014). Bowel endometriosis: colorectal surgeon’s perspective in a multidisciplinary surgical team. World Journal of Gastroenterology: WJG, 20(42), 15616. doi: 10.3748/wjg.v20.i42.15616

Mast cells and endometriosis
Endometriosis is an inflammatory disorder, and this inflammation can lead to increased pain, fatigue, and general feelings of unwellness. Mast cells are immune system cells that can stimulate inflammation (Graziottin, Skaper, & Fusco, 2014). Mast cells hold proinflammatory substances (such as histamine, cytokines, prostaglandins, and more), and, when activated, release these proinflammatory substances (Weller, n.d.). When responding to a threat to the body and for healing, this is a good thing. But when mast cells are activated in endometriosis, not so much.
Activated mast cells (the ones that have released all those proinflammatory substances) have been found in higher quantities in endometriosis lesions versus normal tissue (Hart, 2015; Indraccolo & Barbieri, 2010; Sugamata et al., 2005). Estrogen seems to stimulate mast cells to support the inflammatory process (Zhu et al., 2018). In fact, estrogen receptors are found on mast cells and the high local levels of estrogen from endometriotic lesions may activate the mast cells and lead to pain (Hart, 2015; Zhu et al., 2018). While many therapies for endometriosis involve lowering estrogen production by the feedback loop between the brain and the ovaries, it should be remembered that endometriosis lesions demonstrate production of estrogen themselves (and also show resistance to progesterone) (Delvoux et al., 2009). In fact, the level of estrogen in endometriosis lesions were related to pain symptoms in patients with endometriosis while blood levels of estrogen were not (Zhu et al., 2018).
In addition, nerve fibers in endometriosis lesions have been shown to “release neural peptides such as nerve growth factor and substance P” that in turn activate mast cells to release those proinflammatory substances “which contributes to the development of pain and hyperalgesia in patients with endometriosis” (Zhu & Zhang, 2013). Those granules released by mast cells can contribute to new blood vessel growth, more inflammation, and nerve growth, which can lead to pain (Graziottin, 2009). This persistent inflammation from endometriosis lesions “intensifies neurogenic inflammation and tissue damage” leading to “progressive functional and anatomic damage associated with prominent tissue scarring, exemplified by the natural history of endometriosis” and “up-regulation of nerve pain” (Graziottin, 2009).
So, mast cells are recruited to endometriosis lesions, respond to the higher local estrogen and other inflammatory conditions, release their proinflammatory substances which can lead to pain and scarring. This effect of mast cells is associated in other pain syndromes as well, such as interstitial cystitis, IBS, vulvodynia, complex regional pain syndrome, migraines, and fibromyalgia (Aich et al., 2015).
References
Aich, A., Afrin, L. B., & Gupta, K. (2015). Mast cell-mediated mechanisms of nociception. International journal of molecular sciences, 16(12), 29069-29092. Retrieved from https://doi.org/10.3390/ijms161226151
Delvoux, B., Groothuis, P., D’Hooghe, T., Kyama, C., Dunselman, G., & Romano, A. (2009). Increased production of 17β-estradiol in endometriosis lesions is the result of impaired metabolism. The Journal of Clinical Endocrinology & Metabolism, 94(3), 876-883. Retrieved from https://academic.oup.com/jcem/article/94/3/876/2596530
Graziottin, A., Skaper, S. D., & Fusco, M. (2014). Mast cells in chronic inflammation, pelvic pain and depression in women. Gynecological Endocrinology, 30(7), 472-477. Retrieved from https://www.tandfonline.com/doi/abs/10.3109/09513590.2014.911280
Graziottin, A. (2009). Mast cells and their role in sexual pain disorders. Female Sexual Pain Disorders, 176. Retrieved from https://www.fondazionegraziottin.org/ew/ew_articolo/1820%20-%20mast%20cells%20and%20SPD.pdf
Hart, D. A. (2015). Curbing inflammation in multiple sclerosis and endometriosis: should mast cells be targeted?. International journal of inflammation, 2015. Retrieved from https://www.hindawi.com/journals/iji/2015/452095/
Indraccolo, U., & Barbieri, F. (2010). Effect of palmitoylethanolamide–polydatin combination on chronic pelvic pain associated with endometriosis: Preliminary observations. European Journal of Obstetrics & Gynecology and Reproductive Biology, 150(1), 76-79. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0301211510000424
Sugamata, M., Ihara, T., & Uchiide, I. (2005). Increase of activated mast cells in human endometriosis. American journal of reproductive immunology, 53(3), 120-125. Retrieved from https://doi.org/10.1111/j.1600-0897.2005.00254.x
Weller, C. (n.d.). Mast cells. Retrieved from https://www.immunology.org/public-information/bitesized-immunology/cells/mast-cells
Zhu, T. H., Ding, S. J., Li, T. T., Zhu, L. B., Huang, X. F., & Zhang, X. M. (2018). Estrogen is an important mediator of mast cell activation in ovarian endometriomas. Reproduction, 155(1), 73-83. Retrieved from https://doi.org/10.1530/REP-17-0457
Zhu, L., & Zhang, X. (2013). Research advances on the role of mast cells in pelvic pain of endometriosis. Journal of Zhejiang University (Medical Science), 42(4), 461. DOI: 10.3785/j.issn.1008-9292.2013.04.015

FAQ’s, Podcasts, Resources About Endo, and More!
You can find a diverse gathering of information about endometriosis on our website. We have some information you may not have thought to look for or were unsure of where it might located. Here’s a glimpse at a few of the resources you can find:
In our Resources section, you will find material that includes a wide variety of topics and links to help you on your endometriosis journey.
- If you prefer to listen instead of read, we have several links to podcasts, videos, and webinars.
- If you are looking for info on advocacy and other helpful sources, then see here.
- Need information about navigating insurance? We have info on what to know to help be your own best advocate- as well as info for those on Tricare
- We have topics specific for teens, infertility, pregnancy, and LGBTQIA+
- Tips for topics such as keeping track of your personal medical history, things to pack for surgery/hospital, what to expect before and after surgery, and more.
- Resources for those in the UK and Australia
- and more!
In our Frequently Asked Questions section, you can find answers to questions such as:
- Is that really true? Info on Myths and Misinformation
- Is endometriosis an autoimmune disease?
- Does endometriosis increase my risk of cancer?
- Is There Microscopic or Occult Endometriosis
- Can endometriosis persist after hysterectomy/ovary removal/menopause?
- Is there a genetic component to endometriosis?
- Is there a link between heart disease and endometriosis?
- What effects can long term low estrogen cause?
Endometriosis has several related conditions that can cause similar symptoms. While treating endometriosis is important, it is equally important to treat these other conditions that might be present in order to find relief.
- Adenomyosis
- Endometrial/Uterine Polyps
- Interstitial Cystitis/Bladder Pain Syndrome
- Pelvic Floor Dysfunction
- Fibroids (Leiomyomas)
- Polycystic Ovarian Syndrome (PCOS)
- Pudendal Neuralgia and Vulvodynia
- Pelvic Congestion Syndrome
- Occult Hernia
- Migraines and Endometriosis
Information about endometriosis itself and its treatment can be found throughout the website.
- What makes endometriosis different from the lining of the uterus? Differences in how endometriosis looks and behaves (how it behaves in response to estrogen and progesterone, can make its own nerves and blood vessels, as well as other differences)
- Where can endometriosis be found in the body? (including some weird places)
- How does endometriosis start?
- What are the symptoms of endometriosis?
- How is it diagnosed? How useful are an ultrasound, MRI, or labwork with endometriosis?
- Why is excision surgery recommended? Why should I see a specialist?
- What treatment options are there?
You’ll find all these topics and more on the website. Start exploring!

Your Story Isn’t Over; Mental Health Awareness
May is mental health awareness month and a good time to shine a light on the affects that endometriosis has on our mental health. A significant number of people worldwide suffer from a mental health disorder. While mental health covers a wide spectrum of disorders, two of the most pervasive are anxiety and depression (NAMI, 2021). Both of these not only affect a large portion of the population in general, but also can be found in higher rates in those with chronic illnesses- especially those involving chronic pain (Li et al., 2018).
Endometriosis has been associated “a wide spectrum of different types of pain, ranging from severe dysmenorrhea to chronic pelvic and other comorbid pain conditions” and those with endometriosis have an “elevated likelihood of developing depression and anxiety disorders” (Li et al., 2018). Endometriosis greatly affects quality of life, relationships, stress, professional life, and many other factors that can play into depression and anxiety (Donatti et al., 2017; Lagana et al., 2017). While these factors can play into depression and anxiety, research has suggested that endometriosis leads to specific changes in the brain that are associated with pain, anxiety, and depression (Lima Filho et al., 2019). For example, in a study done on mice, researchers found that “endometriosis led to changes in expression of several genes in the brain regions associated with pain, anxiety, and depression” (Li et al., 2018). In addition, some studies have shown a shared genetic predisposition between depression and endometriosis (Adewuyi et al., 2021).
Our mental health is important. As chronic pelvic pain from endometriosis can affect our mental health, it is important to address the underlying cause (Van den Broeck et al., 2013). But we also need to seek care for our mental health in other ways as well. We can’t do it all alone and seeking help from a professional for our mental health is every bit as important as seeking help for a broken bone. Just as we do physical therapy to help our musculoskeletal system, counseling and cognitive behavioral therapy is like physical therapy for our mental well-being. Endometriosis impacts our relationships, our ability to work, our sense of self, and pretty much every aspect of our lives. Seeking help to cope is not a sign of weakness, but of strength. One of my favorite symbols for mental health is from The Semicolon Project. The semicolon is a sign that the sentence, the story, isn’t over yet. Know that you are not alone, and your story isn’t over yet.
National Suicide Prevention Hotline: 1-800-273-8255
References
Adewuyi, E. O., Mehta, D., Sapkota, Y., Auta, A., Yoshihara, K., Nyegaard, M., … & Nyholt, D. R. (2021). Genetic analysis of endometriosis and depression identifies shared loci and implicates causal links with gastric mucosa abnormality. Human Genetics, 140(3), 529-552. doi: 10.1007/s00439-020-02223-6
Donatti, L., Ramos, D. G., Andres, M. D. P., Passman, L. J., & Podgaec, S. (2017). Patients with endometriosis using positive coping strategies have less depression, stress and pelvic pain. Einstein (São Paulo), 15(1), 65-70. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5433310/
Laganà, A. S., La Rosa, V. L., Rapisarda, A. M. C., Valenti, G., Sapia, F., Chiofalo, B., … & Vitale, S. G. (2017). Anxiety and depression in patients with endometriosis: impact and management challenges. International journal of women’s health, 9, 323. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440042/
Li, T., Mamillapalli, R., Ding, S., Chang, H., Liu, Z. W., Gao, X. B., & Taylor, H. S. (2018). Endometriosis alters brain electrophysiology, gene expression and increases pain sensitization, anxiety, and depression in female mice. Biology of reproduction, 99(2), 349-359. Retrieved from https://doi.org/10.1093/biolre/ioy035
Lima Filho, P. W. L., Chaves Filho, A. J. M., Vieira, C. F. X., de Queiroz Oliveira, T., Soares, M. V. R., Jucá, P. M., … & das Chagas Medeiros, F. (2019). Peritoneal endometriosis induces time-related depressive-and anxiety-like alterations in female rats: involvement of hippocampal pro-oxidative and BDNF alterations. Metabolic brain disease, 34(3), 909-925. Retrieved from https://doi.org/10.1007/s11011-019-00397-1
National Alliance on Mental Illness (NAMI). (2021). Mental health by the numbers. Retrieved from https://www.nami.org/mhstats
Van den Broeck, U., Meuleman, C., Tomassetti, C., D’Hoore, A., Wolthuis, A., Van Cleynenbreugel, B., … & D’Hooghe, T. (2013). Effect of laparoscopic surgery for moderate and severe endometriosis on depression, relationship satisfaction and sexual functioning: comparison of patients with and without bowel resection. Human Reproduction, 28(9), 2389-2397. Retrieved from https://doi.org/10.1093/humrep/det260
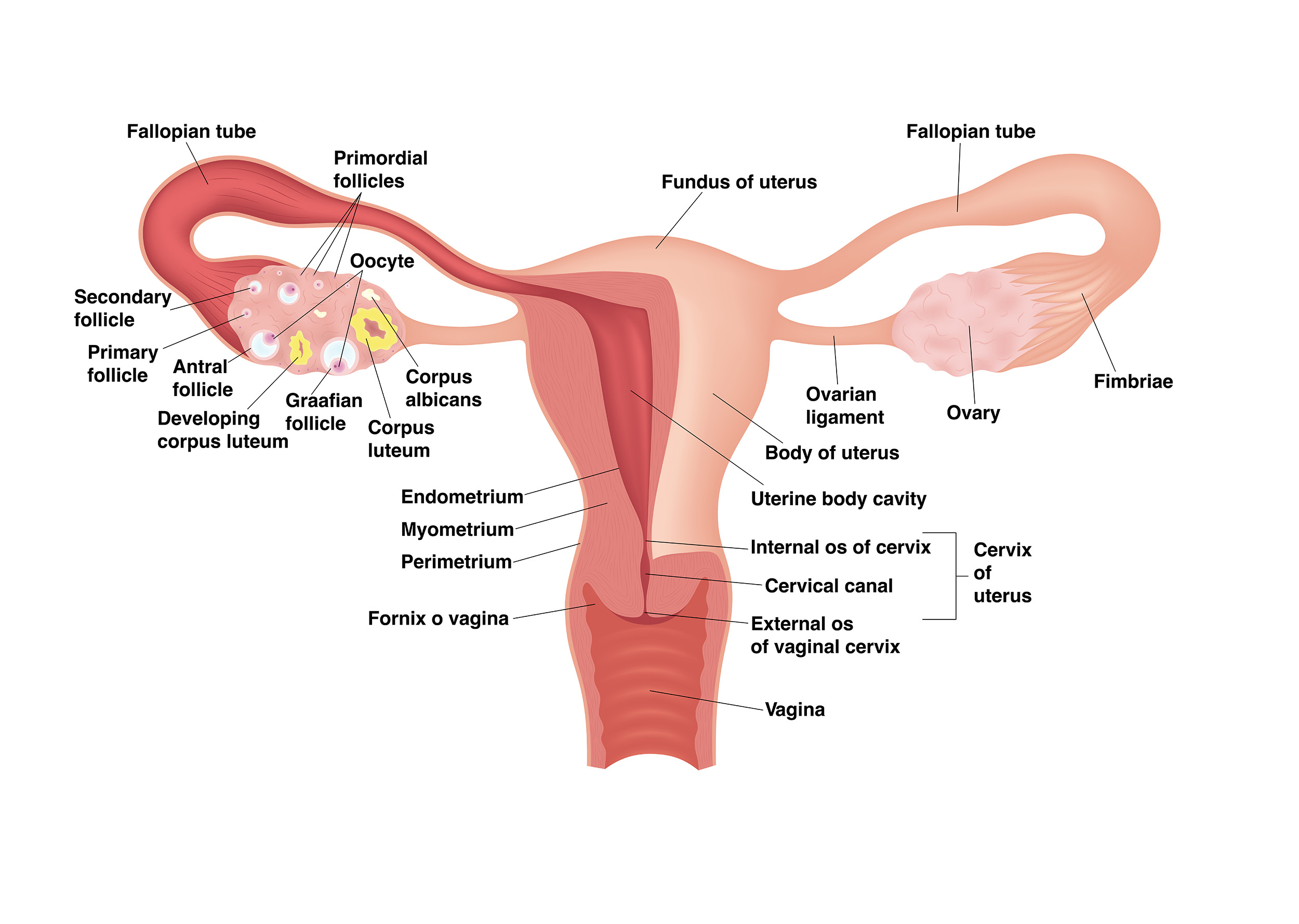
Endometriosis after a hysterectomy or menopause
what are the symptoms of endometriosis after menopause?
Endometriosis does not “die off” or go away with a hysterectomy or menopause. Some people do find some relief from their symptoms, but endometriosis can still persist. Endometriosis often has several related or comorbid conditions (such as adenomyosis or fibroids) that share similar symptoms (pain with menstruation, chronic pelvic pain, etc.) that a hysterectomy might help – but it may not stop your symptoms from endometriosis. Endometriosis exists outside of the uterus and can still respond to hormonal influences (Bulun et al., 2002). Even if your ovaries are removed, endometriosis lesions can produce their own estrogen (Huhtinen et al., 2012). This is important to note because estrogen causes endometriosis lesions to grow and persist (Bulun et al., 2012). So even with the removal of the ovaries or with menopause, endometriosis can sustain itself.
There is high recurrence of symptoms with the removal of just the uterus; but, even with the removal of the ovaries, any endometriosis lesions left behind can continue to grow, progress, and cause symptoms (Clayton et al., 1999; Inceboz, 2015; Khan et al., 2013; Rizk et al., 2014). So, if you have your uterus and ovaries removed for other conditions, it is best that all endometriosis lesions be removed as well. The skill of the surgeon at removing all endometriosis is important. Rizk et al. (2014) report that “the recurrence of endometriosis symptoms and pelvic pain are directly correlated to the surgical precision and removal of peritoneal and deeply infiltrated disease.”
Endometriosis has been found in about 2.2% of postmenopausal women (Zanello et al., 2019). Inceboz (2015) states that “endometriotic lesions remained biologically active, with proliferative activity and preserved hormonal responsiveness, even in the lower estrogenic environment in the postmenopause.” Postmenopausal endometriosis should be managed surgically according to Streuli et al. (2017) and Zanello et al. (2019).
What about hormone replacement if you are in menopause or have had your uterus and ovaries removed? Hormone replacement therapy (HRT) is important as “the hypo-estrogenic state was demonstrated to be a risk factor for cardiovascular and bone disease” (Zanello et al., 2019). While HRT has not been concluded useful for preventing heart disease, it can be useful for those at a higher risk of osteoporosis (Zanello et al., 2019). There isn’t much data available to help guide the decision, but Zanello et al. (2019) report that “in young menopausal women with premature or surgically-induced menopause the benefits of HRT probably overcome the risks” and “in women with residual endometriosis after surgery, the use of HRT should be discussed and the risk of recurrence should be carefully considered before starting an estrogen-based replacement therapy”. Rizk et al. (2014) also states that “the general consensus is that the benefits outweigh the risks” and that starting HRT soon after menopause does not seem to have a faster rate of recurrence. Zanello et al. (2019) concludes that “based on low-grade evidence in the literature, we recommend prescribing combined HRT instead of unopposed estrogen.” It also depends on if your endometriosis was removed.
Does Endometriosis Go Away After Menopause?
endometriosis symptoms after menopause
References
Bulun, S. E., Gurates, B., Fang, Z., Tamura, M., Sebastian, S., Zhou, J., … & Yang, S. (2002). Mechanisms of excessive estrogen formation in endometriosis. Journal of reproductive immunology, 55(1-2), 21-33. Retrieved from https://doi.org/10.1016/S0165-0378(01)00132-2
Bulun, S. E., Monsavais, D., Pavone, M. E., Dyson, M., Xue, Q., Attar, E., … & Su, E. J. (2012, January). Role of estrogen receptor-β in endometriosis. In Seminars in reproductive medicine (Vol. 30, No. 01, pp. 39-45). Thieme Medical Publishers. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4034571/…
Clayton, R. D., Hawe, J. A., Love, J. C., Wilkinson, N., & Garry, R. (1999). Recurrent pain after hysterectomy and bilateral salpingo‐oophorectomy for endometriosis: evaluation of laparoscopic excision of residual endometriosis. BJOG: An International Journal of Obstetrics & Gynaecology, 106(7), 740-744. Retrieved from https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/j.1471-0528.1999.tb08377.x?fbclid=IwAR04aFoLsukqsYutNPNXtJNZpKLNEJbgOOon334NW8D7wvwzZMWaS2YaZts
Huhtinen, K., Ståhle, M., Perheentupa, A., & Poutanen, M. (2012). Estrogen biosynthesis and signaling in endometriosis. Molecular and cellular endocrinology, 358(2), 146-154. Retrieved from https://www.sciencedirect.com/science/article/abs/pii/S0303720711005041
Inceboz, U. (2015). Endometriosis after menopause. Women’s Health, 11(5), 711-715. Retreived from https://journals.sagepub.com/doi/full/10.2217/whe.15.59
Khan, K. N., Kitajima, M., Fujishita, A., Nakashima, M., & Masuzaki, H. (2013). Toll‐like receptor system and endometriosis. Journal of Obstetrics and Gynaecology Research, 39(8), 1281-1292. Retrieved from https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/jog.12117
Rizk, B., Fischer, A. S., Lotfy, H. A., Turki, R., Zahed, H. A., Malik, R., … & Herrera, D. (2014). Recurrence of endometriosis after hysterectomy. Facts, views & vision in ObGyn, 6(4), 219. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4286861/
Zanello, M., Borghese, G., Manzara, F., Degli Esposti, E., Moro, E., Raimondo, D., … & Seracchioli, R. (2019). Hormonal replacement therapy in menopausal women with history of endometriosis: a review of literature. Medicina, 55(8), 477. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6723930/

Endometriosis and Pregnancy
Endometriosis is often associated with infertility. Infertility does not mean you cannot get pregnant, but rather there is a delay in achieving pregnancy. It is technically defined as not achieving a “clinical pregnancy after 12 months or more of regular unprotected sexual intercourse” (World Health Organization, n.d.). An estimated 30–50% of women with endometriosis are reported to have difficulty with infertility (Macer & Taylor, 2012). In addition, endometriosis does not have to be an “advanced stage” for it to affect fertility (Bloski & Pierson, 2008).
“Current evidence indicates that suppressive medical treatment of endometriosis does not benefit fertility and should not be used for this indication alone. Surgery is probably efficacious for all stages of the disease.”
(Ozkan, Murk, & Arici, 2008)
With infertility being related to endometriosis, it is unbelievable that pregnancy might still be recommended as a treatment for endometriosis. While some may have a temporary relief of symptoms, others can experience an increase. In fact, some “imaging and histopathology studies of endometriotic lesions during pregnancy show that they may grow rapidly during pregnancy” (Leeners & Farquhar, 2019). Pregnancy will not treat or cure endometriosis. Research has stated that “women aiming for pregnancy on the background of endometriosis should not be told that pregnancy may be a strategy for managing symptoms and reducing progression of the disease” (Leeners et al., 2018). This is echoed again by Leeners and Farquhar (2019) who point out that “the decision to have children should not be influenced by any perceived benefit of improving endometriosis but should be made solely on the wish for parenthood.”
While the overall risk is still low, endometriosis has been associated with some difficulties during pregnancy. Zullo et al. (2017) looked at 24 studies involving almost 2 million women with endometriosis to consider the possible effects of endometriosis during pregnancy . They found that “women with endometriosis have a statistically significantly higher risk of preterm birth, miscarriage, placenta previa, small for gestational age infants, and cesarean delivery” compared to healthy controls (Zullo et al., 2017). Zullo et al. (2017) did not find any significant association with gestational hypertension and preeclampsia with endometriosis; however, adenomyosis has been found to have some correlation with pregnancy-induced hypertension and preeclampsia (Porpora et al., 2020). Adenomyosis has been found to result in a higher likelihood of preterm birth, small for gestational age, and pre-eclampsia (Razavi et al., 2019). Adenomyosis and endometriosis frequently coexist, so it can be hard to determine how much is one or the other causing these effects (Choi et al., 2017).
On a positive note, Porpora et al. (2020) noted that “no difference in fetal outcome was found” and concluded that “endometriosis does not seem to influence fetal well-being”. This was also found by Uccella et al. (2019), stating that “neonatal outcomes are unaffected by the presence of the disease”. Again, a normal pregnancy is still highly possible. For more information on this topic, see Pregnancy and Endometriosis.
References
Bloski, T., & Pierson, R. (2008). Endometriosis and chronic pelvic pain: unraveling the mystery behind this complex condition. Nursing for women’s health, 12(5), 382-395. doi: 10.1111/j.1751-486X.2008.00362.x
Choi, E. J., Cho, S. B., Lee, S. R., Lim, Y. M., Jeong, K., Moon, H. S., & Chung, H. (2017). Comorbidity of gynecological and non-gynecological diseases with adenomyosis and endometriosis. Obstetrics & gynecology science, 60(6), 579. Retrieved from https://synapse.koreamed.org/upload/SynapseData/PDFData/3021ogs/ogs-60-579.pdf
Leeners, B., Damaso, F., Ochsenbein-Kölble, N., & Farquhar, C. (2018). The effect of pregnancy on endometriosis—facts or fiction?. Human reproduction update, 24(3), 290-299. Retrieved from https://doi.org/10.1093/humupd/dmy004
Leeners, B., & Farquhar, C. M. (2019). Benefits of pregnancy on endometriosis: can we dispel the myths?. Fertility and sterility, 112(2), 226-227. Retrieved from https://doi.org/10.1016/j.fertnstert.2019.06.002
Macer, M. L., & Taylor, H. S. (2012). Endometriosis and infertility: a review of the pathogenesis and treatment of endometriosis-associated infertility. Obstetrics and Gynecology Clinics, 39(4), 535-549. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3538128/pdf/nihms422379.pdf
Ozkan, S., Murk, W., & Arici, A. (2008). Endometriosis and infertility: epidemiology and evidence‐based treatments. Annals of the New York Academy of Sciences, 1127(1), 92-100. DOI: 10.1196/annals.1434.007
Porpora, M. G., Tomao, F., Ticino, A., Piacenti, I., Scaramuzzino, S., Simonetti, S., … & Benedetti Panici, P. (2020). Endometriosis and pregnancy: a single institution experience. International journal of environmental research and public health, 17(2), 401. Retrieved from https://www.mdpi.com/1660-4601/17/2/401
Razavi, M., Maleki‐Hajiagha, A., Sepidarkish, M., Rouholamin, S., Almasi‐Hashiani, A., & Rezaeinejad, M. (2019). Systematic review and meta‐analysis of adverse pregnancy outcomes after uterine adenomyosis. International Journal of Gynecology & Obstetrics, 145(2), 149-157. Retrieved from https://www.endometriozisdernegi.org/konu/dosyalar/pdf/makale_ozetleri/Mayis2019/makale17.pdf
Uccella, S., Manzoni, P., Cromi, A., Marconi, N., Gisone, B., Miraglia, A., … & Ghezzi, F. (2019). Pregnancy after endometriosis: maternal and neonatal outcomes according to the location of the disease. American journal of perinatology, 36(S 02), S91-S98. DOI: 10.1055/s-0039-1692130
World Health Organization. (n.d.).Infertility definitions and terminology. Retrieved from https://www.who.int/teams/sexual-and-reproductive-health-and-research/areas-of-work/fertility-care/infertility-definitions-and-terminology
Zullo, F., Spagnolo, E., Saccone, G., Acunzo, M., Xodo, S., Ceccaroni, M., & Berghella, V. (2017). Endometriosis and obstetrics complications: a systematic review and meta-analysis. Fertility and sterility, 108(4), 667-672. Retrieved from https://doi.org/10.1016/j.fertnstert.2017.07.019

How to Study a Research Study
We post a lot of links and references to research studies, but it can be difficult to interpret them. Even harder is determining how relevant those studies are. Here are a few things to consider as you look at research on endometriosis.
When you look at research studies, you first want to assess how strong of evidence it is presenting. One quick way to tell is by the type of study. The University of Alabama at Birmingham (2021) has a good list of the types of studies, going from strongest evidence to weakest. In short:
“The most scientific, rigorous study designs are randomized controlled trials, systematic reviews, and meta-analysis. These types of studies are thought to provide stronger levels of evidence because they reduce, but do not eliminate, potential biases and confounders.”
(University of Alabama at Birmingham, 2021)
Bias is any errors in design that might throw off the conclusions. Bias, whether intentional or unintentional, can occur in “data collection, data analysis, interpretation and publication which can cause false conclusions” (Simundic, 2013). Find out more about that here. Confounding factors are any variables not factored into the study that can muddle with the interpretation of the results- “they can suggest there is correlation when in fact there isn’t” (Statistics How To, n.d.). This is important when looking at the conclusions drawn. For instance, in last week’s newsletter about endometriomas, we noted that recurrence rates are hard to tell from studies because their definition of “recurrence” varies widely from study to study (was it pathology from surgery or recurrence of symptoms that might actually be from a related condition?). You also want to look how large the study was, did it include several different variables, was it limited to a specific group, how was the study funded and what ethical considerations are given, etc. One tool for helping to analyze such factors can be found here.
Most studies have a short summary at the beginning that can be helpful. For instance, let’s look at this study from Shigesi et al. (2019) found here. The title itself tells us it is a systematic review and meta-analysis: “The association between endometriosis and autoimmune diseases: a systematic review and meta-analysis”. So, we’re starting off good.
The study then starts with the summary called an abstract- which tells us the background of the problem they want to study, how they performed the study, the outcomes they found, and a discussion on what those outcomes mean. In the background, they state that “an association between endometriosis and autoimmune diseases has been proposed”, so that is what they are studying. Then they detail how they are going to study it- what databases they are using to look for information, what they are going to include or exclude from their study, and the statistical analysis they will utilize. They next present the outcomes: “the studies quantified an association between endometriosis and several autoimmune diseases, including systemic lupus erythematosus (SLE), Sjögren’s syndrome (SS), rheumatoid arthritis (RA), autoimmune thyroid disorder, coeliac disease (CLD), multiple sclerosis (MS), inflammatory bowel disease (IBD), and Addison’s disease”. But wait! There is a caveat they note- “the quality of the evidence was generally poor due to the high risk of bias in the majority of the chosen study designs and statistical analyses” and that “only 5 of the 26 studies could provide high-quality evidence”. Then they present their conclusions of how this information might be useful- “the observed associations between endometriosis and autoimmune diseases suggest that clinicians need to be aware of the potential coexistence of endometriosis and autoimmune diseases when either is diagnosed”. They end by giving suggestions for future research that might strengthen the body of evidence for this. In short, after looking deeper into the association, the evidence available is overall poor so more research is warranted.
This is by no means a comprehensive review of looking at research study but rather a brief intro. There are many available resources on the internet for looking more in depth about how to assess research and draw conclusions from it.
References
Shigesi, N., Kvaskoff, M., Kirtley, S., Feng, Q., Fang, H., Knight, J. C., … & Becker, C. M. (2019). The association between endometriosis and autoimmune diseases: a systematic review and meta-analysis. Human reproduction update, 25(4), 486-503. Retrieved from https://academic.oup.com/humupd/article/25/4/486/5518352?login=true
Simundic, A. M. (2013). Bias in research. Biochemia medica, 23(1), 12-15. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3900086/
Statistics How To. (n.d.). Confounding Variable: Simple Definition and Example. Retrieved from https://www.statisticshowto.com/experimental-design/confounding-variable/
University of Alabama at Birmingham. (2021). Study Types- Definitions. Retrieved from https://guides.library.uab.edu/ebd/evidencestrength

