Top Endometriosis Specialist Florida: Your Path to Pain-Free Living
Endometriosis affects approximately 10% of women in Florida, impacting their daily lives and overall well-being. This chronic condition, characterized by the growth of uterine-like tissue outside the uterus, can cause debilitating pain, fertility issues, and a range of other symptoms. For those living in the Sunshine State, an endometriosis specialist is crucial to managing this complex disorder effectively. The persistent pelvic pain, heavy menstrual bleeding, and fatigue associated with the condition can significantly hinder one’s ability to enjoy the state’s beautiful beaches, outdoor activities, and vibrant social scene. Patients can benefit from personalized care plans tailored to their unique needs and lifestyles by choosing an endometriosis specialist in Florida.
As we delve deeper into the world of endometriosis care in Florida, we’ll explore the importance of specialized treatment, highlight top experts in the field, and discuss the various options available to those seeking relief from this challenging condition. Whether you’re newly diagnosed or have been struggling with endometriosis for years, this comprehensive guide will empower you to take control of your health and find your path to pain-free living in the Sunshine State.
Understanding Endometriosis: More Than Just a Sunshine State Struggle
Endometriosis is a complex gynecological condition that affects women worldwide, including those living in Florida. To fully appreciate the importance of seeking specialized care, it’s crucial to understand the intricacies of this disorder and how it impacts the lives of patients.
Decoding the Complexities of Endometriosis
Endometriosis occurs when tissue similar to the lining of the uterus grows outside the uterine cavity. This misplaced tissue can be found on various organs, including the ovaries, fallopian tubes, bladder, and even the intestines. Despite being outside the uterus, this tissue continues to respond to hormonal changes throughout the menstrual cycle, leading to inflammation, pain, and the formation of scar tissue.
The exact cause of endometriosis remains unknown, but several factors may contribute to its development, including:
- Retrograde menstruation
- Genetic predisposition
- Immune system dysfunction
- Environmental factors
Understanding these potential causes is essential for developing effective treatment strategies and managing the condition long-term.
How Endometriosis Affects Floridians’ Active Lifestyles
Florida’s warm climate and abundance of outdoor activities make it an ideal place for an active lifestyle. However, for women with endometriosis, the state’s unique environment can present additional challenges:
- Heat sensitivity: Florida’s hot and humid weather can exacerbate pelvic pain and inflammation associated with endometriosis.
- Beach activities: Swimming and sunbathing, popular pastimes in Florida, may be uncomfortable or even painful for those with severe pelvic pain or bloating.
- Outdoor sports: Engaging in high-impact activities like running or tennis can be challenging due to pelvic discomfort and fatigue.
- Social events: Florida’s vibrant social scene may be difficult to enjoy fully when dealing with unpredictable pain and fatigue.
- Work-life balance: The state’s tourism and service industries often require long hours and physical stamina, which can be taxing for those managing endometriosis symptoms.
Recognizing the Signs of Endometriosis: A Comprehensive Symptom Checklist
Recognizing endometriosis can be difficult due to its wide range of symptoms. To help, here’s a comprehensive checklist of common endometriosis symptoms to watch for:
- Severe menstrual cramps
- Chronic pelvic pain
- Pain during or after sexual intercourse
- Heavy or irregular menstrual bleeding
- Painful bowel movements or urination, especially during menstruation
- Lower back pain
- Abdominal bloating
- Fatigue
- Nausea or vomiting
- Infertility or difficulty conceiving
- Diarrhea or constipation
- Mood swings or depression
- Leg pain
- Painful ovulation
- Chest pain or shortness of breath (in rare cases of thoracic endometriosis)
- Painful urination
It’s important to note that experiencing one or more of these symptoms doesn’t necessarily mean you have endometriosis. However, if you’re concerned about your symptoms, consulting with an endometriosis specialist in Florida can help you receive an accurate diagnosis and appropriate treatment plan.
The Florida Advantage: Cutting-Edge Endo Care Close to Home
Florida offers its residents and visitors a unique advantage regarding endometriosis care. The Sunshine State has become a hub for advanced medical treatments and research, providing women with access to top-tier care without requiring extensive travel. This section explores the benefits of seeking endometriosis treatment in Florida and highlights the state’s commitment to medical excellence in this field.
Access to Top-Tier Treatments and Research
Florida’s medical landscape is characterized by its commitment to innovation and cutting-edge treatments. For women with endometriosis, this translates to:
- Advanced Diagnostic Techniques: Florida’s leading medical centers utilize state-of-the-art imaging technologies, such as high-resolution ultrasounds and MRI scans, to accurately diagnose and stage endometriosis.
- Minimally Invasive Surgical Options: Some Florida specialists are trained in advanced laparoscopic and robotic surgical techniques, offering patients less invasive treatment options with shorter recovery times.
- Participation in Clinical Trials: Several Florida medical institutions actively participate in endometriosis research, allowing patients to access experimental treatments and contribute to scientific advancements.
- Multidisciplinary Approach: Some of Florida’s experts employ a team-based approach, bringing together gynecologists, general surgeons, urologists, pain specialists, fertility experts, and other relevant professionals to provide comprehensive care.
- Fertility Preservation Options: For women concerned about their future fertility, Florida offers advanced reproductive technologies and fertility preservation techniques alongside endometriosis treatment.
Top Endometriosis Specialists in Florida: Experts You Can Trust
Florida is home to some highly skilled and best endometriosis specialists dedicated to providing exceptional care for women struggling with this complex condition. These experts combine their extensive knowledge with cutting-edge techniques to offer personalized treatment plans that address each patient’s unique needs. In this section, we’ll highlight some of the leading endometriosis specialists in Florida and explore their areas of expertise.
Dr. Andrea Vidali is a renowned endometriosis specialist in Miami, Florida, and New York. With over two decades of experience in reproductive endocrinology and infertility, Dr. Vidali has gained international recognition for his expertise in minimally invasive surgical techniques for endometriosis treatment.

Key areas of expertise:
- Advanced excision surgery
- Fertility preservation in endometriosis patients
- Immunological aspects of endometriosis
- Robotic-assisted endometriosis surgery
Dr. Vidali’s approach focuses on thorough diagnosis and comprehensive treatment plans that address both pain management and fertility concerns. His patients benefit from his extensive experience in complex cases and his commitment to staying at the forefront of endometriosis research and treatment innovations.
Dr. Gaby Moawad is a highly respected gynecologist and endometriosis specialist in Orlando, Florida. Known for his patient-centered approach, he combines surgical expertise with a deep understanding of the holistic needs of women with endometriosis.

Areas of specialization:
- Laparoscopic and robotic excision of endometriosis
- Management of chronic pelvic pain
- Fertility-sparing endometriosis treatments
- Multidisciplinary approach to endometriosis care
Dr. Moawad’s practice emphasizes comprehensive care, addressing not only the physical symptoms of endometriosis but also the emotional and psychological aspects of living with a chronic condition. His patients appreciate his compassionate approach and dedication to improving their quality of life.
Finding the right endometriosis specialist in Florida takes time and research. Consultations offer a chance to discuss your case and assess the fit. Choosing the best specialist is key to managing your condition and improving your quality of life, as these experts understand the unique challenges women with endometriosis face in Florida.
Treatment Options: As Diverse as Florida’s Landscape
Just as Florida boasts a diverse landscape of beaches, swamps, and citrus groves, the treatment options for endometriosis in the state are equally varied and comprehensive. Florida’s endometriosis specialists offer a wide range of advanced surgical techniques, non-invasive therapies, and holistic approaches to address the complex needs of patients with this challenging condition. This section explores the diverse treatment landscape available to women seeking endometriosis care in Florida.
Advanced Surgical Techniques Available in Florida
Surgical intervention remains a cornerstone of endometriosis treatment, especially for severe cases or when conservative measures have failed. Florida’s top endometriosis specialists are skilled in various advanced surgical techniques:
- Laparoscopic Excision Surgery:
- A minimally invasive approach using small incisions
- Allows for thorough removal of endometrial implants
- Reduced scarring and faster recovery compared to open surgery
- Often considered the gold standard for endometriosis treatment
- Robotic-Assisted Surgery:
- Utilizes advanced robotic technology for enhanced precision
- Offers 3D visualization and improved dexterity for complex procedures
- Particularly useful for deep-infiltrating endometriosis
- Fertility-Preserving Surgery:
- Focuses on removing endometriosis while preserving reproductive organs
- Often combined with fertility treatments for women trying to conceive
- Presacral Neurectomy:
- Targets nerve pathways to alleviate chronic pelvic pain
- It can be performed alongside excision surgery for comprehensive treatment
- Hysterectomy with Bilateral Salpingo-Oophorectomy:
- Reserved for severe cases or when other treatments have failed
- Involves the removal of the uterus, fallopian tubes, and ovaries
- Considered a last resort due to its impact on fertility and hormonal balance
Non-Invasive Therapies and Holistic Approaches
Florida’s endometriosis specialists recognize the importance of non-surgical interventions and holistic care in managing the condition. Some common non-invasive therapies include:
- Hormonal Treatments:
- Birth control pills
- Progestin-only medications
- GnRH agonists and antagonists
- Aromatase inhibitors
- Pain Management Techniques:
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Nerve blocks
- Transcutaneous electrical nerve stimulation (TENS)
- Physical Therapy:
- Pelvic floor therapy
- Manual therapy techniques
- Exercise programs tailored for endometriosis patients
- Nutritional Counseling:
- Anti-inflammatory diets
- Elimination diets to identify food sensitivities
- Supplementation strategies
- Complementary Therapies:
- Acupuncture
- Yoga and mindfulness practices
- Herbal medicine under professional guidance
- Psychological Support:
- Cognitive-behavioral therapy
- Support groups
- Stress management techniques
Choosing the Right Treatment Plan
When considering endometriosis treatment options in Florida, working closely with your specialist to develop a personalized plan is essential. Factors to consider include:
- Severity and location of endometriosis lesions
- Primary symptoms and their impact on quality of life
- Fertility goals and reproductive health concerns
- Overall health and any coexisting conditions
- Personal preferences and lifestyle considerations
Florida endometriosis specialists offer comprehensive care through a multimodal approach. They combine surgery with noninvasive therapies to address physical and emotional symptoms. With diverse treatment options—from advanced surgery to holistic therapies—patients can access personalized care for effective management and improved quality of life.
Living with Endometriosis in Florida: Beyond Medical Care
Managing endometriosis extends far beyond the doctor’s office or operating room. For those living with this condition in Florida, finding ways to cope with symptoms and maintain a high quality of life is crucial. The Sunshine State’s unique environment and lifestyle offer challenges and opportunities for those navigating life with endometriosis. This section explores strategies for managing symptoms in Florida’s climate and lifestyle and the supportive therapies and resources available to endometriosis patients in the state.
Adapting to Florida’s Climate and Lifestyle
Florida’s warm, humid climate and active lifestyle can present unique challenges for women with endometriosis. Here are some strategies to help manage symptoms while enjoying all that the state has to offer:
- Heat Management:
- Use cooling products like portable fans or cooling towels when outdoors
- Plan outdoor activities for cooler parts of the day
- Stay hydrated to help regulate body temperature
- Beach-Friendly Strategies:
- Invest in comfortable, supportive swimwear
- Use beach umbrellas or tents for shade and privacy
- Bring a supportive cushion or beach chair for comfort
- Exercise Adaptations:
- Opt for low-impact activities like swimming or yoga
- Try water aerobics or beach walks for gentle exercise
- Listen to your body and pace yourself during physical activities
- Workplace Accommodations:
- Use ergonomic furniture to reduce pelvic strain
- Take regular breaks to stretch and move
- Communicate with employers about flexible work arrangements if needed
- Social Life Adjustments:
- Plan activities with built-in rest periods
- Choose venues with comfortable seating options
- Be open with friends about your needs and limitations
Supportive Therapies for Endometriosis Management
Florida offers many supportive therapies that can complement medical treatments and help manage endometriosis symptoms.
- Acupuncture:
- It may help reduce pain and inflammation
- It can be particularly beneficial for menstrual cramps and chronic pelvic pain
- Massage Therapy:
- It helps relax tense muscles and reduce overall body pain
- It may improve circulation and reduce stress
- Yoga and Pilates:
- Gentle stretching can help alleviate pelvic pain
- Mindfulness aspects can aid in stress reduction
- Nutritional Counseling:
- Guidance on anti-inflammatory diets
- Help in identifying and managing food sensitivities
- Pelvic Floor Physical Therapy:
- Addresses muscle tension and dysfunction in the pelvic area
- Can improve pain during intercourse and bladder/bowel symptoms
- Mindfulness and Meditation:
- Techniques for managing pain and reducing stress
- Can improve overall emotional well-being
Community Resources and Support Groups
Florida offers numerous resources and support groups for women living with endometriosis:
- Endometriosis Association of Florida:
- Provides education and support for patients and families
- Organizes regular meetups and events across the state
- Online Support Communities:
- Florida-specific Facebook groups and forums
- Virtual support meetings for those unable to attend in-person events
- Fertility Support Networks:
- Resources for women dealing with endometriosis-related infertility
- Connections to fertility specialists and treatment options in Florida
- Workplace Advocacy Groups:
- Organizations that help women navigate workplace challenges related to chronic illness
- Resources for understanding employment rights and accommodations
Lifestyle Modifications for Symptom Management
In addition to medical treatments and supportive therapies, certain lifestyle modifications can help manage endometriosis symptoms:
- Stress Reduction Techniques:
- Regular meditation or deep breathing exercises
- Engaging in hobbies or activities that promote relaxation
- Sleep Hygiene:
- Establishing a consistent sleep schedule
- Creating a comfortable sleep environment
- Dietary Adjustments:
- Keeping a food diary to identify trigger foods
- Incorporating anti-inflammatory foods into the diet
- Exercise Routine:
- Finding a balance between rest and gentle activity
- Incorporating low-impact exercises like swimming or cycling
- Emotional Well-being:
- Seeking counseling or therapy to address the emotional impact of living with a chronic condition
- Practicing self-compassion and setting realistic expectations
By using Florida’s resources and strategies, women with endometriosis can manage symptoms and maintain a fulfilling lifestyle. Remember, it’s a journey—be patient and celebrate small victories.
Conclusion: Empowering Your Endo Journey in the Sunshine State
As we conclude our exploration of endometriosis care in Florida, it’s clear that the Sunshine State offers a wealth of resources, expertise, and support for women navigating this challenging condition. From world-class specialists to cutting-edge treatments and supportive communities, Florida provides a comprehensive ecosystem for endometriosis management. We encourage you to take the next step in your endometriosis care journey. Whether that means scheduling a consultation with a specialist, exploring new treatment options, or connecting with a local support group, every action you take is a step towards better health and well-being.
Remember, your health journey is unique, and finding the right care may take time. Be patient with yourself, advocate for your needs, and don’t hesitate to seek second opinions or explore different treatment options. With perseverance and the right support, you can navigate the challenges of endometriosis and embrace all that life in Florida has to offer.
Here’s to your health, well-being, and a brighter, pain-free future in the Sunshine State!
REFERENCES:
https://ufhealth.org/conditions-and-treatments/endometriosis
https://www.medicalnewstoday.com/provider-near-me/condition-or-procedure/endometriosis/fl-florida
https://www.acibademhealthpoint.com/endometriosis-specialist-in-miami-expert-care
https://health.usf.edu/care/obgyn/services-specialties/endometriosis

Endometriosis Pain? Discover the Best OB-GYN Near You for Expert Care
Living with Endometriosis: Why Finding the Right OB-GYN Near You Matters
Living with endometriosis can be an overwhelming and isolating experience. Chronic pain, heavy periods, and potential fertility issues can significantly impact your quality of life. However, you don’t have to face this challenging condition alone. Finding a skilled and compassionate endometriosis OB-GYN near you who can make all the difference in managing your symptoms effectively and regaining control of your health.
In this comprehensive guide, we’ll explore the importance of seeking specialized care for endometriosis, how to identify the right OB-GYN in your area, and what to expect from treatment. Whether you’ve been diagnosed recently or have struggled with endometriosis for years, this article will empower you to take the next step toward finding relief and improving your overall well-being.
What Is Endometriosis and Why Your OB-GYN Matters
Endometriosis is a complex gynecological condition that affects millions of women worldwide. It occurs when tissue similar to the lining of the uterus grows outside the uterine cavity, commonly on the ovaries, fallopian tubes, and pelvic lining. This misplaced tissue responds to hormonal changes during the menstrual cycle, leading to inflammation, pain, and scar tissue formation.
The symptoms of endometriosis can vary widely from person to person but often include:
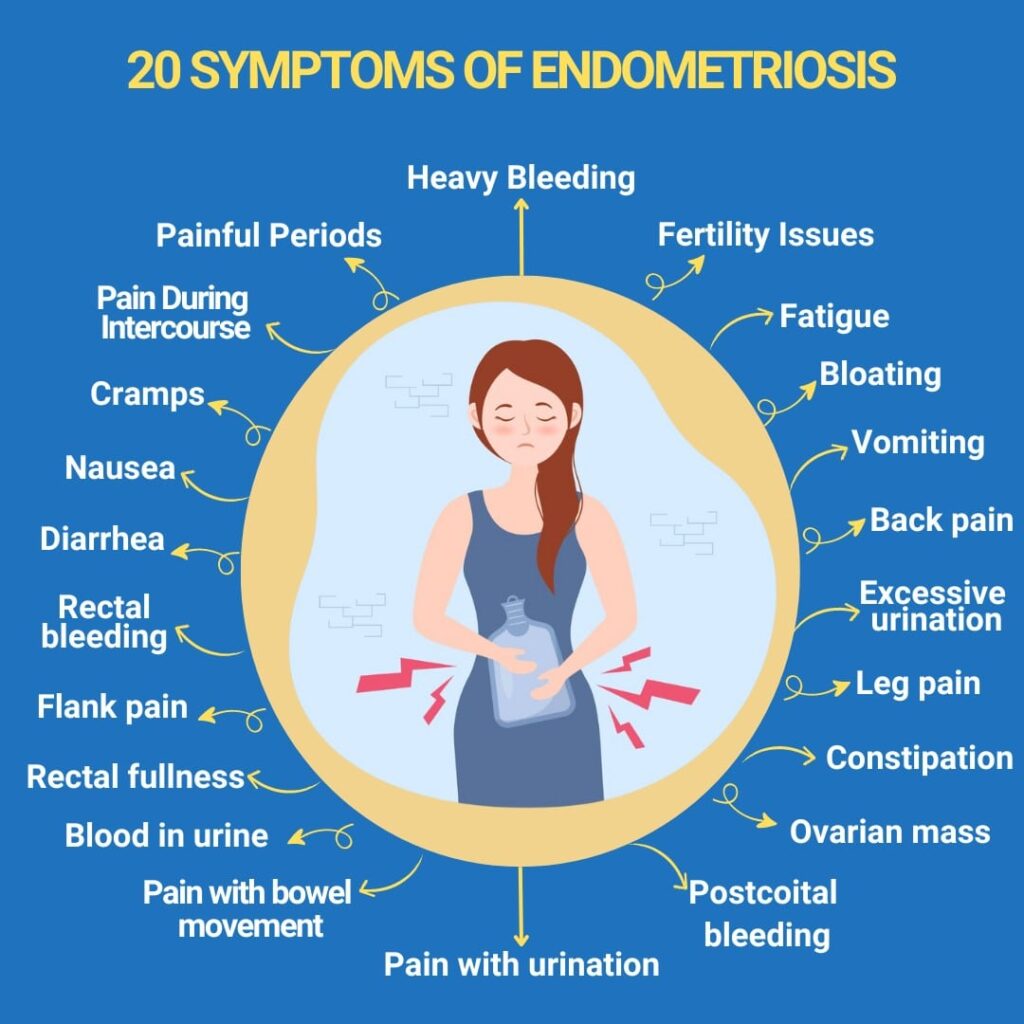
- Severe menstrual cramps that worsen over time
- Chronic pelvic pain
- Pain during or after sexual intercourse
- Heavy or irregular menstrual bleeding
- Painful bowel movements or urination during menstruation
- Fatigue and gastrointestinal issues
- Difficulty conceiving or infertility
Endometriosis is very complex. There is a general lack of knowledge and expertise among doctors, including OB-GYNs, in diagnosing and treating patients. Therefore, seeking care from an OB-GYN with specialized knowledge and experience in treating endometriosis is crucial. These experts are better equipped to provide accurate diagnoses, develop personalized treatment plans, and offer the latest advancements in endometriosis care.
How to Identify the Best OB-GYN Doctor for Endometriosis Near You
Finding the right OB-GYN doctor specializing in endometriosis requires research and consideration. You should use these strategies to locate the best specialist near you:
Utilize Online Resources and Directories
Several online platforms can help you find experienced endometriosis specialists in your area. One such resource is iCareBetter, a directory designed to connect patients with skilled endometriosis surgeons and specialists. This endometriosis specialist directory provides detailed information about the doctor’s experience, patient reviews, and areas of expertise.
Seek Referrals from Trusted Sources
Don’t hesitate to ask for recommendations from:
- Your primary care physician
- Your physical therapist, dietitian, yoga teacher, counselor, and nurses.
- Friends or family members who have dealt with endometriosis
- Local endometriosis support groups
- Online communities dedicated to endometriosis awareness and support
Research Credentials and Experience
When evaluating potential OB-GYNs, consider the following factors:
- Board certification in obstetrics and gynecology
- Additional fellowship training or specialization in minimally invasive GYN surgery and endometriosis, such as AAGL fellowship
- Years of experience treating endometriosis patients
- Membership in professional organizations focused on endometriosis research and treatment, such as AAGL
- Publications or involvement in clinical trials related to endometriosis
Read Patient Reviews and Testimonials
While individual experiences may vary, patient reviews can provide valuable insights into a doctor’s bedside manner, communication style, and overall patient satisfaction. Look for patterns in feedback and consider both positive and negative reviews to form a balanced perspective. You can read endometriosis-specific patient reviews on doctors’ profiles on iCareBetter.com.
Schedule Consultations
Many OB-GYNs offer initial consultations to discuss your symptoms and concerns. This is an excellent opportunity to assess their approach to endometriosis care and determine if you feel comfortable with their communication style and treatment philosophy.
Comprehensive Treatment Approaches Offered by Endometriosis Specialists
Experienced OB-GYNs specializing in endometriosis recognize that every patient’s journey is unique and requires a personalized treatment approach. Top-tier endometriosis surgeons offer multidisciplinary surgery and care. These experts include Dr. Andrea Vidali, Dr. Steven Vasilev, Dr. Amanda Chu, Dr. Lora Liu, Dr. Ken Sinervo, and many more surgeons who, in total, add up to about one hundred experts in the US. Here are some of the most common approaches used by endometriosis specialists:

Pain Management Strategies
Managing chronic pain is often a top priority for endometriosis patients. Endometriosis surgeons may recommend a combination of:
- Surgery
- Over-the-counter pain relievers (NSAIDs)
- Prescription pain medications
- Physical therapy and pelvic floor exercises
- Alternative therapies such as acupuncture or mindfulness techniques
Hormonal Therapies
Hormonal treatments aim to temporarily manage endometriosis symptoms or regulate your hormones before and after surgery. Options may include:
- Combined oral contraceptives
- Progestin-only medications
- Gonadotropin-releasing hormone (GnRH) agonists or antagonists
- Aromatase inhibitors
Minimal Invasive Surgical Procedures
Surgical intervention may be necessary for more severe cases or when conservative treatments are ineffective. Skilled endometriosis specialists often employ advanced laparoscopic techniques to:
- Remove endometrial implants and scar tissue
- Restore normal pelvic anatomy
- Preserve fertility when possible
Integrative and Holistic Approaches
Many endometriosis specialists recognize the benefits of combining conventional surgical and medical treatments with complementary therapies. These may include:
- Nutritional counseling and anti-inflammatory diets
- Stress reduction techniques
- Pelvic floor physical therapy
- Cognitive-behavioral therapy for pain management
- Pain management by pain specialists or acupuncturists
Fertility Preservation and Treatment
For patients concerned about their fertility, endometriosis specialists work closely with you to develop strategies for preserving and enhancing fertility. This may involve:
- Fertility-sparing surgical techniques
- Ovarian stimulation and egg-freezing
- In vitro fertilization (IVF) when necessary
- Egg preservation before surgery
The Benefits of Early Intervention by a Skilled OB-GYN
Seeking care from an experienced endometriosis specialist near you as early as possible can have numerous benefits for your overall health and quality of life.
- Accurate and timely diagnosis: Endometriosis can be challenging to diagnose, and patients may need about 10 years to receive a firm diagnosis. However, specialists are trained to recognize subtle signs and symptoms that general practitioners may overlook.
- Preventing disease progression: Early intervention can help slow the growth of endometriosis implants and minimize the formation of scar tissue, potentially preserving fertility and reducing long-term complications.
- Tailored treatment plans: Specialists can develop personalized treatment strategies that address your specific symptoms, concerns, and goals.
- Improved pain management: Early intervention can improve pain control and reduce the need for more invasive treatments in the future.
- Enhanced fertility outcomes: For those hoping to conceive, early treatment can help preserve fertility and improve the chances of a successful pregnancy.
- Better overall quality of life: By addressing symptoms early on, you can minimize the impact of endometriosis on your daily activities, relationships, and emotional well-being.
Why Proximity Matters in Choosing an Endometriosis Specialist Near You
When dealing with a chronic condition like endometriosis, having a trusted healthcare provider close to home can make a significant difference in your overall treatment experience and outcomes. Here are some key reasons why proximity matters when choosing an OB-GYN for endometriosis care:
- Convenience and accessibility: Check-ups and follow-up appointments are essential for effectively managing endometriosis. Having a specialist nearby reduces travel time and makes it easier to maintain consistent care.
- Timely intervention: In case of flare-ups or emergencies, being able to quickly reach your OB-GYN can provide peace of mind and ensure prompt medical attention.
- Familiarity with local resources: A local specialist is likely to have established relationships with other healthcare providers in the area, facilitating seamless referrals for additional treatments or support services if needed.
- Community support: Choosing a local OB-GYN may connect you with other patients in your area, fostering a sense of community and shared experiences.
- Continuity of care: Building a long-term relationship with a nearby specialist allows for more personalized and comprehensive care over time.
Start your search today with terms like “endometriosis OB-GYN near me” to find a trusted expert in your area who can provide personalized, timely care. However, because of a significant shortage of skilled endometriosis experts, with an estimated 100 experts in the US, you might end up traveling. In that case, virtual visits will be your best friend.
FAQs About Seeing an Endometriosis OB-GYN Near You
Once you’ve found an OB-GYN specializing in endometriosis, preparing for your initial consultation is important. Here are some tips to help you make the most of your appointment:
- Keep a symptom diary: Record your symptoms, their frequency, and severity in the weeks leading up to your appointment. This information can help your doctor better understand your condition.
- Gather your medical history: Compile a list of any previous diagnoses, treatments, and surgeries related to your pelvic pain and reproductive health.
- Bring relevant medical records: If you’ve had imaging studies or lab tests done previously, bring copies of the results to your appointment.
- Prepare a list of questions: Write down any concerns or questions you have about your symptoms, diagnosis, or treatment options.
- Consider bringing a support person: Having a friend or family member with you can provide emotional support and help you remember important information discussed during the appointment.
Essential Questions to Ask Your Endometriosis Specialist
During your consultation, don’t hesitate to ask questions that will help you better understand your condition and treatment options. Some important endometriosis FAQs to consider:
- What stage of endometriosis do you suspect I have, and how can we confirm the diagnosis?
- What treatment options do you recommend for my specific case, and why?
- What are the potential side effects or risks associated with each treatment option?
- How will the recommended treatments affect my fertility?
- Are there any lifestyle changes or complementary therapies you suggest to help manage my symptoms?
- What is your experience with treating endometriosis, and how many similar cases have you handled?
- How often should I schedule follow-up appointments, and what signs should prompt me to contact you between visits?
- Are there any clinical trials or new treatments for endometriosis that I might be eligible for?
Understanding Insurance Coverage for Endometriosis Treatment
Navigating insurance coverage for endometriosis treatment can be complex. Here are some key points to keep in mind:
- Most health insurance plans cover diagnostic tests and basic treatments for endometriosis.
- Coverage for more advanced treatments, such as laparoscopic surgery or fertility treatments, may vary depending on your specific plan and the specialist you plan to visit.
- Some insurance providers may require a referral from your primary care physician before covering specialist visits.
- Certain treatments, like experimental therapies or some complementary approaches, may not be covered by insurance.
It is essential to review your insurance policy and contact your provider to understand your coverage details. Your chosen OB-GYN’s office may also be able to assist you in determining coverage and obtaining necessary pre-authorizations for treatment.
Taking the Next Step: Finding Relief with the Right OB-GYN
Living with endometriosis can be challenging, but with the right care and support, you can manage your symptoms effectively and improve your quality of life. By seeking out a skilled OB-GYN who specializes in endometriosis, you’re taking a crucial step towards better health and well-being.
Remember, you don’t have to face this journey alone. Reach out to local support groups, connect with online communities, and most importantly, don’t hesitate to seek professional help. With the guidance of an experienced endometriosis specialist, you can develop a personalized treatment plan that addresses your unique needs and goals.
Take action today to find the best endometriosis OB-GYN near you. Use online resources like iCareBetter, ask for referrals and schedule consultations to find the right specialist who can provide the comprehensive care you deserve. Your path to relief and improved health begins with finding the right healthcare partner. Don’t wait—visit iCareBetter to find the best endometriosis OB-GYN near you today and reclaim your health!
References:
https://www.northwell.edu/obstetrics-and-gynecology/conditions/endometriosis
https://www.brighamandwomens.org/obgyn/resources/endometriosis-treatment
https://www.medifind.com/conditions/endometriosis/1797/doctors
https://www.woosterhospital.org/exploring-nearby-endometriosis-treatment-options
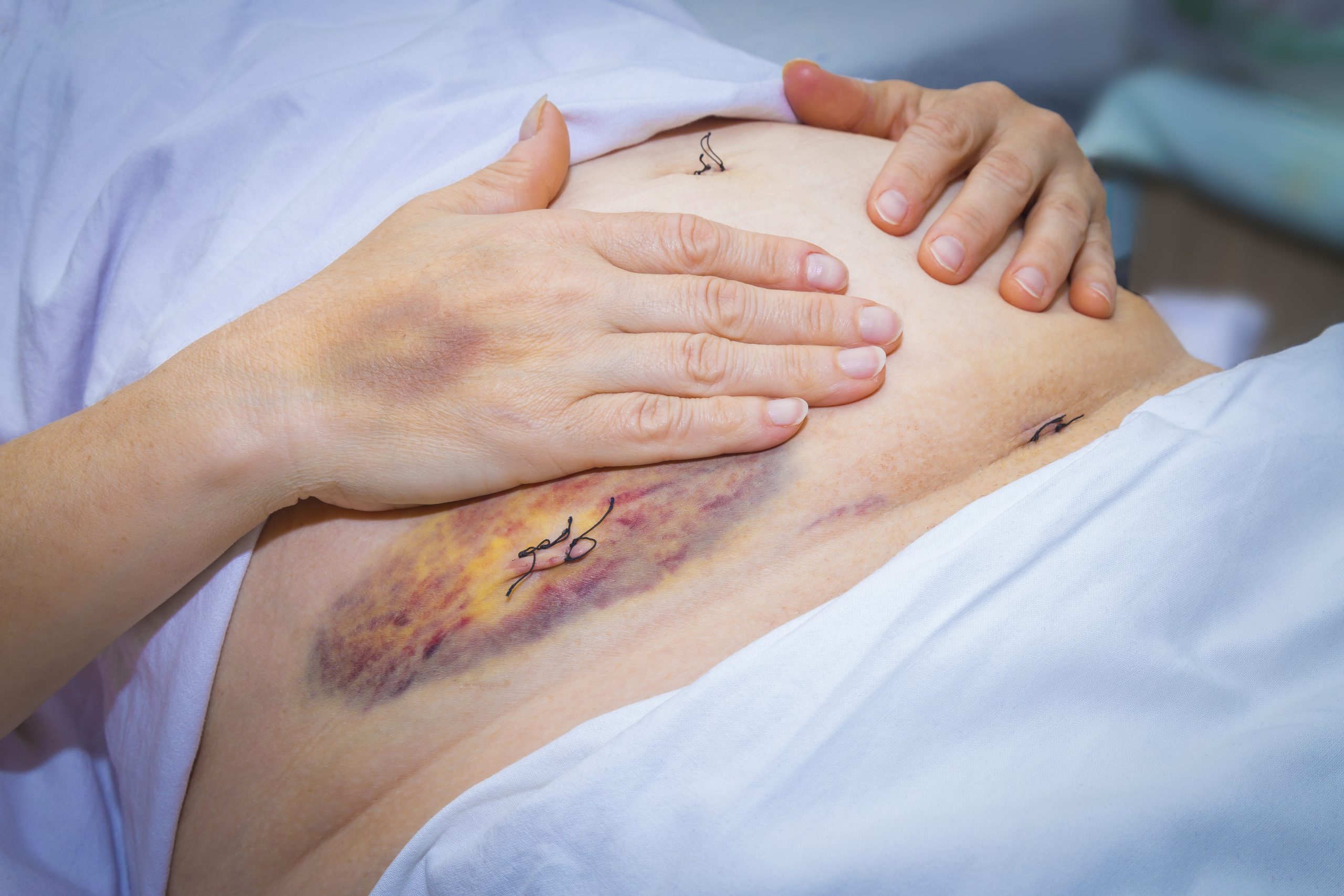
Decoding the Mystery of Scar Endometriosis
Endometriosis, a perplexing condition where endometrial-like tissue is found outside the uterus, manifests in various forms. Among them is scar endometriosis, a rare yet distressing subtype that warrants heightened awareness and understanding. This is often a consequence of surgical procedures. Scar endometriosis can profoundly impact an individual’s quality of life, necessitating prompt diagnosis and effective management.
Table of contents
- Introduction
- Etiology: Unveiling the Root Causes
- Clinical Manifestations: Recognizing the Signs
- Diagnostic Approach: Piecing Together the Puzzle
- Treatment Strategies: Alleviating the Burden
- Preventive Measures: Minimizing the Risk
- Psychological Impact and Support
- Fertility Considerations
- Emerging Treatments and Research Frontiers
- Multidisciplinary Care: A Collaborative Approach
- Patient Education and Advocacy
- Conclusion
Introduction
Scar endometriosis, an extrapelvic manifestation of endometriosis, is characterized by the growth of endometrial-like tissue within or around a surgical scar. While its incidence is relatively low, ranging from 0.03% to 1.08% of endometriosis cases, the symptoms can be just as debilitating and the diagnosis challenging. This article delves into the intricacies of scar endometriosis, shedding light on its causes, symptoms, diagnosis, and treatment options, empowering individuals to navigate this intricate condition with knowledge and confidence.
Etiology: Unveiling the Root Causes
The precise etiology of scar endometriosis remains a subject of ongoing research and debate. However, several theories have been proposed to explain its development:
- Iatrogenic Transplantation: This widely accepted theory suggests that during surgical procedures, endometriosis cells inadvertently become implanted within the surgical incision or scar tissue. This phenomenon is particularly common in obstetric and gynecological surgeries, such as cesarean sections, hysterectomies, and laparoscopic procedures.
- Lymphatic or Vascular Dissemination: Similar to other forms of endometriosis found in the body, these cells may travel through lymphatic or vascular channels, eventually seeding and proliferating within surgical scars or distant sites.
- Metaplastic Transformation: This theory proposes that specialized cells within the surgical scar undergo metaplastic changes, transforming into endometrial-like cells under the influence of specific hormonal or environmental factors.
While these theories provide plausible explanations, the exact mechanisms underlying scar endometriosis remain elusive, underscoring the need for further research to unravel the complexities of this condition.
Clinical Manifestations: Recognizing the Signs
The clinical manifestations of scar endometriosis can vary, making early recognition a challenge. However, certain symptoms may raise suspicion and prompt further investigation:
- Cyclical Pain: One of the hallmark symptoms is cyclical pain or discomfort at the surgical scar site, often coinciding with menstrual periods. This pain can range from mild to severe and may radiate to adjacent areas.
- Swelling or Lump: Many people with scar endometriosis report the presence of a palpable lump or swelling at the scar site. This lump may fluctuate in size and tenderness throughout the menstrual cycle.
- Cyclical Bleeding: In some cases, patients may experience cyclical bleeding or discharge from the surgical scar, further indicating the presence of endometriosis.
- Dysmenorrhea and Pelvic Pain: Scar endometriosis can coexist with pelvic endometriosis, leading to additional symptoms such as dysmenorrhea (painful periods) and chronic pelvic pain, especially if endometriosis has been left untreated.
It is crucial to note that the absence of cyclical symptoms does not necessarily exclude the possibility of scar endometriosis, as some cases may present with non-cyclical pain or discomfort.
Diagnostic Approach: Piecing Together the Puzzle
Diagnosing scar endometriosis can be challenging due to its non-specific symptoms and the need for a multidisciplinary approach. The diagnostic process typically involves the following steps:
- Medical History and Physical Examination: A thorough medical history, including details of previous surgeries, menstrual patterns, and associated symptoms, is essential. During the physical examination, healthcare professionals may palpate the surgical scar site for any palpable masses, nodules, or tenderness.
- Imaging Modalities: Various imaging techniques can aid in the diagnosis and assessment of scar endometriosis:
- Ultrasonography: Ultrasound is often the initial imaging modality employed, as it can detect hypoechoic or heterogeneous lesions with irregular borders at the scar site.
- Magnetic Resonance Imaging (MRI): MRI provides detailed information about the extent and depth of the lesion, aiding in surgical planning.
- Computed Tomography (CT) Scan: While less commonly used, CT scans can help differentiate scar endometriosis from other conditions, such as hernias or malignancies.
- Biopsy and Histopathological Examination: Ultimately, a definitive diagnosis requires a biopsy or surgical excision of the lesion, followed by histopathological examination. The presence of endometrial glands and stroma within the scar tissue confirms the diagnosis of scar endometriosis.
It is essential to note that a multidisciplinary team including gynecologists, radiologists, and pathologists may be necessary to establish an accurate diagnosis and develop an appropriate treatment plan.
Treatment Strategies: Alleviating the Burden
The management of scar endometriosis aims to alleviate symptoms, prevent recurrence, and preserve fertility when desired. The treatment approach is multifaceted and tailored to each individual’s unique circumstances:
- Surgical Intervention: Wide surgical excision with clear margins is the ideal treatment for scar endometriosis. This procedure involves the complete removal of the endometriosis lesion(s), including any affected surrounding tissue or muscle layers. In cases of extensive involvement, abdominal wall reconstruction with mesh reinforcement may be recommended.
- Hormonal Therapy: While not a definitive treatment, hormonal therapies such as oral contraceptives, progestins, or gonadotropin-releasing hormone (GnRH) agonists can provide temporary symptom relief, and some research shows that these therapies may suppress the growth of lesions. However, these medications may have side effects and do not address the underlying lesion.
- Combined Approach: In some cases, a combined approach involving surgical excision followed by adjuvant hormonal therapy may be recommended and may reduce the risk of recurrence.
- Pain Management: Effective pain management strategies, including the use of non-steroidal anti-inflammatory drugs (NSAIDs) or other analgesics, may be necessary to alleviate discomfort associated with scar endometriosis.
It is crucial to engage in shared decision-making with healthcare professionals, weighing the risks and benefits of each treatment option to determine the most appropriate course of action.
Preventive Measures: Minimizing the Risk
While the complete prevention of scar endometriosis may not be feasible in all cases, certain measures can be taken to reduce the risk of its development:
- Meticulous Surgical Technique: During surgical procedures, particularly those involving the uterus or pelvic region, strict adherence to meticulous surgical techniques is paramount. This includes minimizing the risk of cell seeding, proper handling of surgical specimens, and thorough irrigation of the surgical site.
- Containment of Tissue Biopsies: The use of endo-bags or containment devices during laparoscopic procedures can help prevent the inadvertent dissemination of endometriosis cells into the surgical field.
- Careful Wound Closure: Ensuring proper closure of the peritoneum and fascial layers during abdominal surgeries can help minimize the risk of endometriosis cell implantation within the surgical site.
- Postoperative Monitoring: Regular follow-up and vigilance for any signs or symptoms of scar endometriosis in the postoperative period can aid in early detection and prompt management.
While these preventive measures cannot guarantee the complete elimination of scar endometriosis, they can contribute to reducing the risk and promoting better outcomes for patients undergoing surgical procedures.
Psychological Impact and Support
Scar endometriosis can have a profound impact on an individual’s psychological well-being, often leading to feelings of frustration, anxiety, and diminished self-esteem. The chronic pain, discomfort, and potential impact on fertility can take a toll on mental health, underscoring the importance of holistic care and support.
Healthcare professionals should be attuned to the psychological needs of patients with scar endometriosis and provide access to counseling, support groups, or mental health resources as needed. Building a strong support system and fostering open communication can empower an individual to cope with the challenges of this condition more effectively.
Fertility Considerations
For individuals desiring fertility, the impact of scar endometriosis on fertility is a significant concern. While the condition itself may not directly affect fertility, the presence of pelvic endometriosis or the surgical interventions required for treatment can potentially impact fertility outcomes.
In such cases, a multidisciplinary approach involving reproductive endocrinologists and fertility specialists may be necessary. Fertility preservation techniques, such as egg or embryo freezing, may be considered for people undergoing extensive surgical procedures. Ongoing monitoring and tailored treatment plans can help optimize fertility outcomes for those affected by scar endometriosis.
Emerging Treatments and Research Frontiers
While current treatment modalities for scar endometriosis have shown promising results, ongoing research efforts aim to further enhance our understanding and management of this condition. Some emerging areas of interest include:
- Targeted Therapies: The development of targeted therapies that selectively inhibit the growth or proliferation of endometriosis could potentially offer more effective and less invasive treatment options.
- Stem Cell Therapy: Preliminary research explores the potential of stem cell therapy in regenerating or repairing damaged tissue, potentially reducing the need for extensive surgical interventions.
- Genetic and Molecular Studies: Investigating the genetic and molecular mechanisms underlying scar endometriosis could provide insights into its pathogenesis and pave the way for personalized treatment strategies.
- Improved Diagnostic Techniques: Ongoing efforts to refine imaging modalities and develop novel biomarkers could enhance the accuracy and timeliness of scar endometriosis diagnosis.
As research continues to advance, the future holds promise for more effective, personalized, and minimally invasive approaches to managing scar endometriosis.
Multidisciplinary Care: A Collaborative Approach
Scar endometriosis often requires a multidisciplinary approach involving various healthcare professionals, each contributing their expertise to ensure comprehensive care. This collaborative team may include:
- Gynecologists: Gynecologists play a pivotal role in diagnosing, treating, and managing scar endometriosis, as well as addressing any associated pelvic endometriosis or fertility concerns.
- Radiologists: Radiologists are essential in interpreting imaging studies and guiding the diagnostic process, particularly in cases where surgical intervention is being considered.
- Pathologists: Pathologists provide crucial insights by examining tissue samples and confirming the diagnosis of scar endometriosis through histopathological analysis.
- Surgeons: Surgical specialists, such as general surgeons or plastic surgeons, may be involved in the surgical management of scar endometriosis, particularly in cases requiring complex reconstructive procedures or mesh reinforcement.
- Pain Management Specialists: Chronic pain associated with scar endometriosis may necessitate the involvement of pain management specialists to develop effective pain control strategies.
- Mental Health Professionals: Psychologists, counselors, or therapists can provide invaluable support in addressing the psychological impact of scar endometriosis and promoting overall well-being.
Effective communication and collaboration among this multidisciplinary team are essential to ensure comprehensive, coordinated care tailored to each patient’s unique needs.
Patient Education and Advocacy
Empowering patients through education and advocacy is crucial in addressing the challenges posed by scar endometriosis. Healthcare professionals should prioritize providing accurate and up-to-date information to patients, fostering a better understanding of the condition, its implications, and available treatment options.
Patient support groups and advocacy organizations play a vital role in raising awareness, promoting research, and advocating for improved access to care and resources. These platforms can also serve as a valuable source of support, allowing individuals with scar endometriosis to connect, share experiences, and gain strength from one another. By fostering a collaborative approach between healthcare professionals, patients, and advocacy groups, we can collectively work towards improving the quality of life for those affected by scar endometriosis and advancing our understanding of this complex condition.
Conclusion
Scar endometriosis, a rare and often overlooked manifestation of endometriosis, presents unique challenges in diagnosis and management. However, by raising awareness, promoting early recognition, and embracing a multidisciplinary approach, we can better support everyone affected by this condition.
Through meticulous surgical techniques, targeted therapies, and ongoing research, we can strive to alleviate the physical and emotional burdens associated with scar endometriosis. Additionally, fostering open dialogue, patient education, and advocacy efforts can empower an individual to navigate this journey with knowledge, support, and resilience. By unraveling the enigma of scar endometriosis, we can pave the way for more effective treatments, improved quality of life, and a deeper understanding of this intricate condition, ultimately providing hope and solace to those affected.
REFERENCES:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2851454
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10024799
https://www.shreeivfclinic.com/endometriosis/scar-endometriosis
https://casereports.bmj.com/content/2014/bcr-2014-206693
https://www.mdpi.com/2296-3529/9/2/20

Does Removing Endometriosis and Fibroid Tumor Increase the Chances of Pregnancy?
Table of contents
- Overview of Endometriosis and Fibroids
- Endometriosis and Infertility
- Fibroids and Fertility
- Endometriosis and Pregnancy Outcomes
- Fibroids and Pregnancy Outcomes
- Treatment Options for Fertility Preservation
- Fertility Outcomes After Surgery
- Pregnancy Monitoring and Management
- Non-Surgical Treatment Options
- Emerging Treatments and Future Directions
- Emotional and Psychological Support
- Conclusion
Overview of Endometriosis and Fibroids
Endometriosis and uterine fibroids are prevalent gynecological conditions that can profoundly impact a woman’s reproductive health and fertility. Endometriosis, affecting approximately 10% of individuals assigned female at birth (AFAB), occurs when endometrial-like tissue is found outside of the uterus, primarily in the abdominopelvic cavity. Fibroids, on the other hand, are non-cancerous growths made up of fibrous tissue and smooth muscle cells that develop in or around the uterus. They may also be called uterine myomas or leiomyomas and affect an estimated 20–40% of AFABs, often during their childbearing years.
While these conditions are distinct, they share some common characteristics, including the potential to cause infertility and pregnancy complications. This article aims to provide a comprehensive understanding of the effects of endometriosis and fibroids on pregnancy, as well as the various treatment options available to maintain fertility.
Endometriosis and Infertility
Endometriosis is a leading cause of infertility, responsible for approximately 50% of infertility cases. The condition can impair fertility by obstructing the fallopian tubes, disrupting the hormonal milieu, causing inflammation, and altering endometrial development, thereby reducing the chances of successful embryo implantation.
However, it’s important to note that many individuals with endometriosis can still conceive naturally or with the assistance of fertility treatments. The impact of endometriosis on fertility may depend on the severity and location of the endometrial lesions.
Fibroids and Fertility
While fibroids are generally non-cancerous, their presence can affect fertility in several ways. Submucosal fibroids, which protrude into the uterine cavity, can significantly reduce the chances of successful embryo implantation and pregnancy rates during assisted reproductive technologies (ART) such as in vitro fertilization (IVF).
Intramural fibroids, which grow within the uterine muscle wall, can also impair fertility by distorting the uterine cavity and disrupting the hormonal environment necessary for successful implantation and placentation.
Endometriosis and Pregnancy Outcomes
People with endometriosis may face an increased risk of certain adverse pregnancy outcomes, including:
- Placental abnormalities (placenta previa, placental abruption)
- Preterm birth
- Pregnancy-induced hypertension/preeclampsia
- Cesarean delivery
The risk of these complications may be influenced by factors such as the severity of endometriosis, the presence of infertility, and the use of fertility treatments. However, many individuals with endometriosis can have successful, uncomplicated pregnancies.
Fibroids and Pregnancy Outcomes
Fibroids can also impact pregnancy outcomes in various ways. Individuals with fibroids may be at an increased risk of:
- Placental abnormalities (placental abruption, placenta previa)
- Preterm labor and delivery
- Fetal malpresentation (breech presentation)
- Cesarean delivery
- Postpartum hemorrhage
The risk of these complications may be influenced by factors such as the size, number, and location of the fibroids. Large fibroids, or those located in the uterine cavity, may pose a greater risk to the pregnancy.
Treatment Options for Fertility Preservation
For individuals with endometriosis or fibroids who desire future fertility, surgery or removal of the endometriosis lesions and/or fibroid(s) may be recommended to improve their chances of conception and reduce the risk of pregnancy complications.
Endometriosis Surgery
While there is no one-size-fits all approach to addressing endometriosis, surgical excision or removal of the lesions is thought to be the ideal approach to addressing the lesions directly. This minimally invasive surgery aims to remove the lesions while preserving the uterus and ovaries, allowing for future fertility.
Fibroid Removal
For individuals with fibroids who wish to maintain their fertility, a myomectomy may be recommended. This surgical procedure involves the removal of fibroids while preserving the uterus. Depending on the size, number, and location of the fibroids, myomectomies can be performed through various approaches, including:
- Hysteroscopic myomectomy (for submucosal fibroids)
- Laparoscopic myomectomy (for intramural or subserosal fibroids)
- Abdominal myomectomy (for larger or multiple fibroids)
The choice of approach depends on factors such as the size and location of the fibroids, as well as the surgeon’s expertise and the patient’s preferences.
Fertility Outcomes After Surgery
Studies have shown that those who undergo endometriosis excision or myomectomy for fibroid removal can achieve pregnancy rates ranging from 50-60%. However, it’s important to note that these procedures do not guarantee fertility, and the success rates may vary depending on factors such as age, severity of the condition, and the presence of other infertility factors.
Pregnancy Monitoring and Management
For those with endometriosis or fibroids who become pregnant, close monitoring and specialized care may be recommended to mitigate potential risks and ensure the best possible outcomes for both the mother and the baby.
This may involve regular ultrasound examinations to monitor fetal growth and placental function, as well as close monitoring for signs of preterm labor or other complications. In some cases, additional interventions or precautions may be necessary, such as bed rest, medication, or early delivery.
Non-Surgical Treatment Options
While surgical tumor removal is often the preferred option for those seeking to preserve fertility, there are also non-surgical treatment options available for managing endometriosis and fibroids. These include:
Endometriosis:
- Hormonal therapies (e.g., birth control pills, GnRH agonists)
- Anti-inflammatory medications
- Complementary therapies (e.g., dietary modifications, exercise)
Fibroids:
- Gonadotropin-releasing hormone (GnRH) agonists
- Selective progesterone receptor modulators (SPRMs)
- Uterine artery embolization (UAE)
- Magnetic resonance-guided focused ultrasound (MRgFUS)
These non-surgical options may be used to manage symptoms, reduce tumor size, or provide temporary relief before pursuing fertility treatments or tumor removal surgery.
Emerging Treatments and Future Directions
Research is ongoing to develop new and improved treatment options for endometriosis and fibroids, with a particular focus on preserving fertility and minimizing the risk of adverse pregnancy outcomes.
Some areas of active research include:
- Novel hormonal therapies and targeted therapies for endometriosis
- Improved surgical techniques for myomectomy and endometriosis excision
- Non-invasive tumor removal methods (e.g., MRgFUS, UAE)
- Preventative strategies to reduce the risk of endometriosis and fibroid development
As our understanding of these conditions continues to evolve, it is hoped that more effective and less invasive treatment options will become available, improving the quality of life and reproductive outcomes for individuals affected by endometriosis and fibroids.
Emotional and Psychological Support
The journey through endometriosis, fibroids, and infertility can be emotionally and psychologically challenging for many. It’s essential to recognize and address the emotional impact of these conditions, as well as the stress and anxiety that can accompany fertility treatments and pregnancy complications.
Support groups, counseling, and mental health resources can be invaluable in helping individuals cope with the emotional and psychological aspects of their condition and treatment. Healthcare providers should be mindful of these needs and provide appropriate referrals and support services as needed.
Conclusion
Endometriosis and fibroids are common gynecological conditions that can have a significant impact on fertility and pregnancy outcomes. While these conditions can pose challenges, there are various surgical and non-surgical options and treatment strategies available to help individuals achieve their desired family size while mitigating potential risks.
By working closely with their healthcare providers, people with endometriosis or fibroids can develop personalized treatment plans that address their individual needs and preferences. With proper management and care, those suffering from these conditions can successfully navigate pregnancy and achieve their dreams of parenthood.
REFERENCES:
https://www.webmd.com/women/uterine-fibroids/what-if-i-have-uterine-fibroids-while-pregnant
https://www.acfs2000.com/fibroids-and-endometriosis.html
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3608270
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9187594

Navigating the Road to Recovery: A Comprehensive Guide to Endometriosis Surgery Aftercare
The journey towards relief from endometriosis often involves surgical intervention, but the road to recovery can be a winding one. While endometriosis surgery offers hope for alleviating debilitating symptoms, the post-operative phase demands patience, diligence, and a steadfast commitment to self-care. This comprehensive guide aims to equip you with the knowledge and strategies necessary to navigate the recovery process with confidence and ease.
Table of contents
- Understanding the Endometriosis Surgery Landscape
- Preparing for the Post-Operative Journey
- The First Few Days: Taking It Slow
- The Weeks Ahead: Gradual Progress and Patience
- Returning to Normal Activities: Listening to Your Body
- Embracing a Holistic Approach to Recovery
- Addressing Potential Complications and Recurrence
- Fertility Considerations After Endometriosis Surgery
- Embracing a Positive Mindset and Self-Care
- Endometriosis Surgery Recovery: A Transformative Journey
Understanding the Endometriosis Surgery Landscape
Endometriosis, a chronic condition characterized by the growth of endometrial-like tissue outside the uterus, can wreak havoc on an individual’s quality of life. When medications and lifestyle modifications fail to provide adequate relief, surgical intervention may become a viable option. Minimally invasive approaches are now the go-to approaches for endometriosis surgery.
Laparoscopy: A Minimally Invasive Marvel
Laparoscopy, a minimally invasive procedure, is the preferred approach for endometriosis surgery. This technique involves making small incisions in the abdomen and inserting a laparoscope—a slender camera—to visualize and remove endometrial lesions or scar tissue. Laparoscopy offers numerous advantages, including reduced recovery time, minimal scarring, and a lower risk of complications.
Robotic Surgery: A More Advanced Approach
While you may hear mixed opinions on whether robotic surgery is better or worse than a laparoscopic approach, it appears that robotics are the way of the future. Providers using a robotic approach have to undergo more extensive surgical training, but the outcomes may be superior. While the operative time, or time and anesthesia, can be longer than laparoscopic surgeries, the visualization is undoubtedly better. Endometriosis can present with some hard-to-see or hard-to-recognize lesion types, and using this approach may be a better way to visualize those hard-to-see lesions to remove them.
Laparotomy: The Open Approach
This is an older approach that has been replaced with minimally invasive approaches, but you may still occasionally see someone undergo a laparotomy. In cases of extensive endometriosis or when laparoscopy is not feasible, laparotomy, an open surgical procedure, may be recommended. Laparotomy involves a larger incision in the abdomen, allowing for better visualization and access to deeply infiltrating endometriosis lesions. While more invasive, laparotomy may be necessary in certain circumstances.
Preparing for the Post-Operative Journey
Before embarking on the recovery path, it is crucial to lay the groundwork for a smooth transition. Your healthcare provider will provide specific instructions tailored to your unique situation, but here are some general guidelines:
- Arrange Transportation: Have a trusted friend or family member available to drive you home after the procedure, as you will be unable to operate a vehicle immediately following surgery.
- Stock Up on Essentials: Ensure your pantry and refrigerator are stocked with easily digestible foods, such as soups, broths, yogurt, and fruits, as well as plenty of fluids to stay hydrated.
- Prepare for Medication Management: Discuss any necessary medication adjustments with your healthcare provider, including pain relievers, antibiotics, and laxatives to aid in post-operative recovery.
- Create a Comfortable Environment: Arrange your living space to minimize unnecessary movement and exertion, ensuring easy access to essential items and a comfortable resting area.
The First Few Days: Taking It Slow
The initial days following endometriosis surgery are crucial for initiating the healing process. During this time, it is essential to prioritize rest and follow your healthcare provider’s instructions diligently:
- Manage Pain and Discomfort: Take prescribed pain medications as directed to alleviate discomfort and promote healing. Applying a heating pad or ice pack to the incision site can also provide relief.
- Stay Hydrated and Nourished: Consume plenty of fluids and easily digestible foods to support your body’s recovery efforts. Avoid heavy, greasy, or spicy meals that may cause digestive discomfort.
- Embrace Gentle Movement: While rest is essential, light movement, such as short walks around the house, can aid in circulation and prevent complications like blood clots.
- Monitor Incision Sites: Keep an eye on your incision sites for signs of infection, such as redness, swelling, or pus drainage. Follow your healthcare provider’s instructions for proper wound care.
The Weeks Ahead: Gradual Progress and Patience
As the days turn into weeks, your body will continue its healing journey. During this phase, it is important to strike a balance between rest and gentle activity, while adhering to your healthcare provider’s recommendations:
- Increase Activity Levels Gradually: After the initial recovery period, you can gradually increase your activity levels, starting with light exercises like walking or gentle stretching. Listen to your body and avoid overexertion.
- Manage Expectations: Recovery timelines can vary significantly based on the extent of the surgery, your overall health, and individual healing rates. Be patient and celebrate small victories along the way.
- Attend Follow-up Appointments: Keeping scheduled follow-up appointments with your healthcare provider is crucial for monitoring your progress and addressing any concerns or complications that may arise.
- Seek Support: The recovery process can be emotionally and physically taxing. Reach out to loved ones, support groups, or mental health professionals for encouragement and guidance during this journey.
Returning to Normal Activities: Listening to Your Body
As you continue to heal, the desire to resume your normal routine may become increasingly strong. However, it is essential to listen to your body and follow your healthcare provider’s advice regarding the appropriate timeline for returning to various activities:
- Work and School: Depending on the nature of your job or studies, you may be able to return to work or school within two weeks of the surgery. However, if your responsibilities involve physical labor or strenuous activity, a longer recovery period may be necessary.
- Exercise and Sports: Low-impact exercises like walking or light yoga can typically be resumed within a few weeks, but strenuous activities and high-impact sports should be avoided until your healthcare provider gives the green light.
- Intimate Relationships: It is generally recommended to abstain from sexual activity for at least six weeks after endometriosis surgery to allow for proper healing. Discuss any concerns with your healthcare provider.
- Travel and Vacations: While short trips may be possible within a few weeks, it is advisable to postpone extended travel or vacations until you have fully recovered, typically within 6-8 weeks after the surgery.
Embracing a Holistic Approach to Recovery
Recovery from endometriosis surgery extends beyond physical healing; it encompasses emotional and mental well-being as well. Embracing a holistic approach can enhance your overall recovery experience:
- Prioritize Stress Management: Chronic stress can hinder the healing process. Incorporate relaxation techniques like deep breathing exercises, meditation, or gentle yoga into your routine to promote a calm and peaceful mindset.
- Seek Emotional Support: Endometriosis can take a toll on mental health, and the recovery process can be emotionally taxing. Lean on your support system, join support groups, or consider seeking professional counseling to navigate the emotional challenges.
- Nourish Your Body: A balanced diet rich in whole foods, antioxidants, and anti-inflammatory nutrients can aid in the healing process and promote overall well-being. Consult with a nutritionist or dietitian for personalized dietary recommendations.
- Stay Positive and Patient: Recovery from endometriosis surgery is a journey, and setbacks or slower progress than anticipated can be disheartening. Maintain a positive mindset, celebrate small victories, and trust in the healing process.
Addressing Potential Complications and Recurrence
While endometriosis surgery aims to alleviate symptoms and improve quality of life, it is important to be aware of potential complications and the possibility of recurrence:
- Recognizing Signs of Complications: Be vigilant for signs of infection, excessive bleeding, or worsening pain, and promptly report any concerns to your healthcare provider. Especially around the incision sites, look for abnormal redness, swelling, heat, or pain.
- Managing Recurrence Risk: Endometriosis can recur after surgery, even with the best surgery. However, the persistence of endometriosis can occur when not all lesions are removed. Discuss long-term management strategies with your healthcare provider.
- Exploring Alternative Treatments: If endometriosis symptoms persist or recur despite surgery, explore alternative treatment options such as hormonal therapy, pain management techniques, or complementary therapies in consultation with your healthcare provider.
Fertility Considerations After Endometriosis Surgery
For many individuals with endometriosis, preserving fertility is a significant concern. Endometriosis surgery can potentially improve fertility outcomes, but it is crucial to have an open dialogue with your healthcare provider about your goals and options:
- Timing for Conception: Depending on the extent of the surgery and your overall health, your healthcare provider may recommend waiting a specific period before attempting conception to allow for complete healing.
- Assisted Reproductive Technologies: In cases of moderate to severe endometriosis, assisted reproductive technologies (ART), such as in vitro fertilization (IVF), may be recommended to improve pregnancy chances.
- Fertility Preservation Options: If you are considering future fertility but are not ready for conception immediately after surgery, discuss fertility preservation options like egg freezing with your healthcare provider.
Embracing a Positive Mindset and Self-Care
The recovery journey after endometriosis surgery can be physically and emotionally challenging, but embracing a positive mindset and prioritizing self-care can make a significant difference:
- Celebrate Small Victories: Recovery is a process, and every milestone, no matter how small, deserves celebration. Acknowledge and appreciate your progress, even on days when it may seem insignificant.
- Practice Self-Compassion: Be kind and patient with yourself throughout the recovery process. Healing takes time, and setbacks are a natural part of the journey. Treat yourself with the same compassion you would extend to a loved one.
- Engage in Enjoyable Activities: While rest is essential, engaging in low-impact activities that bring you joy and relaxation can boost your mood and overall well-being. Read a book, listen to music, or indulge in a favorite hobby that doesn’t strain your recovery.
- Seek Professional Support: If you find yourself struggling with anxiety, depression, or other mental health concerns during the recovery process, don’t hesitate to seek professional support from a therapist or counselor.
Endometriosis Surgery Recovery: A Transformative Journey
Recovering from endometriosis surgery is a transformative journey that requires patience, perseverance, and a commitment to self-care. While the road may be winding, embracing a positive mindset, following your healthcare provider’s guidance, and listening to your body’s needs can pave the way for a successful recovery and improved quality of life. Remember, every person’s journey is unique, and with the right support and strategies, you can navigate this path with resilience and emerge stronger on the other side.
REFERENCES:
https://my.clevelandclinic.org/health/treatments/4620-endometriosis-surgery
https://www.healthline.com/health/endotough/surgery-for-endometriosis
Understanding Endometriosis and Stomach Cramps
Endometriosis is a medical condition that affects approximately 10% of women globally. Its symptoms can be debilitating and significantly impact the quality of life of those affected. One of the most commonly reported symptoms of endometriosis is stomach cramps. This article delves into the relationship between endometriosis and stomach cramps, unraveling the causes, symptoms, and available treatment options.
Table of contents
What is Endometriosis?
Endometriosis is a health disorder that occurs when tissue similar to the uterus’s endometrium begins to grow in areas outside the uterus. These areas may include the ovaries, fallopian tubes, the lining of the pelvic cavity, and, in some cases, the bowels and bladder.
What is Endo Belly?
One term that has gained popularity in endometriosis discussions is “endo belly.” This term refers to the painful abdominal bloating often associated with endometriosis. The bloating, which can be severe, results from inflammation, growths, gas, or other digestive issues related to endometriosis.
Causes of Endo Belly
The exact cause of endo belly still needs to be fully understood. However, several factors have impacted this symptom. The endometrial-like tissue behaves similarly to the endometrium: it thickens, breaks down, and bleeds with each menstrual cycle. However, since this tissue cannot exit the body, it becomes trapped, leading to inflammation and irritation. Over time, this can cause scar tissue to form, leading to various symptoms, including bloating and fluid retention.
Symptoms of Endo Belly
The primary symptom of endo belly is severe bloating, particularly during or just before the menstrual period. The abdomen may fill with air or gas, causing it to appear larger and feel stiff or tight to the touch. This bloating may last for a few hours to a few weeks. Other symptoms that may accompany endo belly include:
- Nausea and vomiting
- Gas pain
- Constipation or diarrhea
- Abdominal discomfort, pain, and pressure
How Endometriosis Causes Stomach Cramps
The stomach cramps associated with endometriosis are often severe and debilitating. These cramps are not merely due to the menstrual cycle but are a direct result of the endometrial-like tissue growing outside the uterus. This tissue resembles the endometrium, building up and breaking down each menstrual cycle. But because this tissue is outside the uterus and cannot exit the body, it gets trapped. This trapped tissue leads to inflammation and irritation, which can cause severe stomach cramps.
Symptoms of Stomach Cramps Due to Endometriosis
The main symptom associated with endometriosis-induced stomach cramps is severe pain, particularly during the menstrual period. This pain can be so intense that it disrupts daily activities and significantly impairs the individual’s quality of life. The pain often worsens throughout the day and can be so severe that the person may not be able to button their pants or may even appear as though they are pregnant.
Treatment for Endometriosis and Stomach Cramps
There are several treatment options available for managing endometriosis and its associated stomach cramps. Treatment choice often depends on the severity of the symptoms, the person’s age, and their future pregnancy plans. The treatment options include:
- Over-the-counter Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or aspirin, may be recommended to manage inflammation and reduce pain.
- Prescription Hormonal Medications: Hormonal pills or devices may help to regulate symptoms.
- Endometriosis Surgery: In severe cases, surgery may be the best option for long-term pain relief. This surgery involves removing the endometriosis and scar tissue from the pelvic and abdominal organs.
When to Consult a Doctor
It’s essential to consult an endo specialist if you’re experiencing severe stomach cramps, mainly if they’re associated with your menstrual cycle. Early diagnosis and treatment can significantly improve your quality of life and prevent potential complications, such as infertility.
Conclusion
Endometriosis and stomach cramps are closely linked. The condition can lead to severe stomach cramps that can significantly impair the quality of life of those affected. However, you can manage the symptoms effectively with proper diagnosis and treatment. Suppose you’re experiencing severe stomach cramps, especially if they’re associated with your menstrual cycle. In that case, it’s essential to consult a healthcare provider for a proper diagnosis and treatment plan.
References:
https://maidenmedical.com/endometriosis-belly
https://www.healthline.com/health/endo-belly
https://www.endofound.org/gastrointestinal-distress