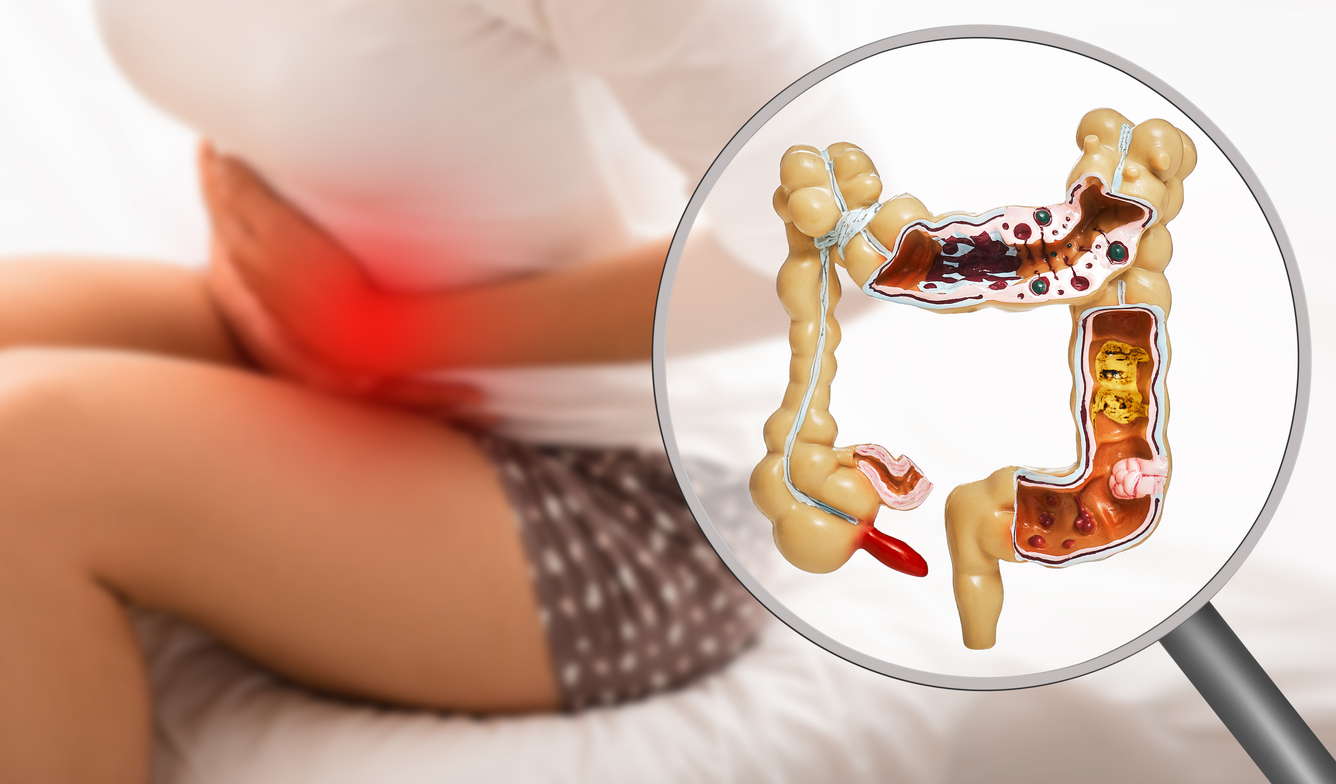
Does Gastrointestinal Endometriosis Cause Infertility
Gastrointestinal endometriosis is a condition that poses numerous health challenges to women, and one of the most concerning questions revolves around its potential impact on fertility. The primary focus of this article is to address the question:
Does gastrointestinal endometriosis cause infertility?
We will dissect this issue by exploring the available medical and scientific evidence.
Understanding Endometriosis and its Symptoms
Endometriosis can manifest with various symptoms, although not all women may experience them. Some common symptoms include:
- Painful periods: Women with endometriosis often experience more intense pelvic pain and cramping before and during their menstrual cycle.
- Chronic lower back/abdominal pain: Another hallmark of endometriosis is persistent pain in the lower back or abdomen.
- Infertility: Endometriosis has been associated with fertility problems, making it more challenging for some women to conceive.
- Excessive bleeding and spotting: Women with endometriosis may experience heavy bleeding during their periods or irregular bleeding between periods due to the presence of adenomyosis.
- Pain during or after intercourse: Endometrial tissue growths can cause pain during sexual intercourse, which can have a significant impact on a woman’s quality of life.
- Gastrointestinal issues: Endometriosis affecting the intestines can lead to symptoms such as painful bowel movements, diarrhea, constipation, and stomach issues like nausea.
- Fatigue: Chronic fatigue is a common complaint among women with endometriosis, which can be attributed to the physical and emotional toll of dealing with the condition.
Endometriosis and Fertility
The relationship between endometriosis and fertility has been a subject of continuous research. Women with endometriosis, particularly moderate to severe forms, often face fertility challenges. However, it’s important to note that endometriosis does not automatically lead to infertility. Many women with endometriosis can and do conceive naturally or with the help of fertility treatments.
How Endometriosis Impacts Fertility
The mechanism through which endometriosis affects fertility is complex and multifaceted. Here are some ways it can potentially interfere with conception:
- Anatomical Distortions: Endometriosis can cause adhesions or scar tissue formation, leading to a distortion of pelvic anatomy. This can block the fallopian tubes or alter the position of the ovaries, hindering the meeting of sperm and egg.
- Inflammatory Environment: Endometriosis creates an inflammatory environment in the pelvic region, which might harm the quality of eggs or sperm and hinder their movement.
- Impact on the Endometrium: Some studies suggest that endometriosis may affect the lining of the uterus (the endometrium), making it less receptive to an implanting embryo.
Gastrointestinal Endometriosis and Infertility: Is there a Connection?
When it comes to the specific question – does gastrointestinal endometriosis cause infertility – the answer is not as straightforward as one might hope. While endometriosis is known to affect fertility in general, the impact of gastrointestinal endometriosis on fertility is less clear.
Evidence suggests that endometriosis involving the bowel or bladder can be more challenging to treat and may require more complex surgical procedures, which could potentially affect reproductive function. However, it’s also important to remember that the presence of gastrointestinal endometriosis does not necessarily mean that a woman will experience fertility problems. However, the inflammation and molecular impacts of endometriosis might still increase the risk of fertility problems.
Treating Gastrointestinal Endometriosis
Medical Treatment
The first line of treatment for endometriosis often involves hormone therapy, such as birth control pills or progestin-based contraceptives, which work by managing symptoms and manipulating hormones. However, these medications do not improve fertility.
Surgical Treatment
Surgery to remove endometriosis patches can potentially improve fertility, especially in cases of moderate to severe endometriosis. However, surgical treatment of gastrointestinal endometriosis can be complex and may carry a higher risk of complications. Depending on the extent of the disease, it may involve resection of a portion of the bowel or bladder.
The Path to Pregnancy with Endometriosis
Surgical treatment can increase the chance of natural and assisted fertility. However, in many cases the patient still needs further support and treatment.
Fertility Treatments
For women with endometriosis who are struggling to conceive, assisted reproductive technologies (ART) such as in-vitro fertilization (IVF) may be an option. While women with severe endometriosis may have a lower success rate with IVF than other women, many are still able to achieve a successful pregnancy with this treatment.
Surrogate pregnancy
There are some options to seek help from other women’s bodies and eggs if necessary and desired.
Maintaining Hope
The journey of dealing with endometriosis and its potential impact on fertility can be emotionally challenging. However, it’s important to maintain hope. Many women with endometriosis, including gastrointestinal endometriosis, are able to conceive and have healthy pregnancies, whether naturally or with the help of fertility treatments.
Final Thoughts
In conclusion, while gastrointestinal endometriosis can pose challenges, it can impact fertility by inflammation and molecular pathways. Each case of endometriosis is unique, and the impact on fertility can vary greatly from one individual to another. If you’re dealing with endometriosis and are concerned about your fertility, it’s important to seek guidance from a healthcare provider who can provide individualized advice based on your specific situation.
Remember, understanding your condition and exploring your options can empower you to make the best decisions for your health and fertility journey. So, while gastrointestinal endometriosis can pose hurdles, they are not insurmountable. With the right treatment and support, the dream of parenthood can still be a reality for many women living with endometriosis.
References:
https://pubmed.ncbi.nlm.nih.gov/32631683/
https://www.obgyn-care.net/blog/does-endometriosis-cause-infertility
https://www.nhs.uk/conditions/endometriosis/complications/

How Common is Infertility with Endometriosis
Endometriosis, a medical condition affecting women globally, often poses a significant question:
how common is infertility with endometriosis? This article aims to shed light on this critical question, discussing endometriosis and its relationship with fertility issues, the possible causes and treatments, and the hope that exists for women battling both endometriosis and infertility.
Understanding Endometriosis
Endometriosis is a chronic disorder characterized by the growth of endometrial-like tissue (the lining of the uterus) outside the uterus, inducing a chronic inflammatory reaction. This misplaced tissue can be found on the ovaries, fallopian tubes, and even on the bladder or intestines. The growths can lead to complications, including the formation of scar tissue and cysts, causing pain and potentially affecting fertility.
Read More: Can Endometriosis Be Treated Without Surgery? – Endometriosis Supportive Therapy
Prevalence of Endometriosis
Endometriosis affects an estimated 10–15% of women between 15-50. However, the prevalence dramatically rises to about 25%–50% in women with infertility. Despite the well-supported association between endometriosis and infertility, a causal relationship is yet to be definitively established.
Endometriosis and Infertility: The Connection
Endometriosis can impact fertility in multiple ways, leading to the following complications:
- Impact on Gametes and Embryos: The increased number of inflammatory cells in the peritoneal fluid of women with endometriosis can damage the oocytes (eggs) and sperm and even have toxic effects on the embryo.
- Impairment of Fallopian Tubes and Ovarian Function: Endometriosis can lead to pelvic adhesions, blocked fallopian tubes, and damaged ovaries, which can hinder the process of ovulation and egg release, thus affecting fertility.
- Endometrial Receptivity: The chronic inflammatory state induced by endometriosis can impair endometrial receptivity, affecting the implantation of a pregnancy.
Read More: Can Minimal Endometriosis Cause Infertility
Endometriosis-Associated Infertility: Treatment Approaches
The treatment for endometriosis-associated infertility usually involves a combination of medical and surgical interventions. The choice of treatment depends on several factors, including the age of the woman, the severity of the symptoms, the desire for pregnancy, and the extent of the disease.
Medical Treatment
Medical treatments for endometriosis aim to suppress the growth of endometriosis tissue and relieve symptoms. These treatments include hormonal therapies such as birth control pills, gonadotropin-releasing hormone (GnRH) agonists, and progestins. However, these treatments do not improve fertility rates and are typically used to alleviate pain and other symptoms. They are temporary solutions.
Surgical Treatment
Surgical treatment aims to remove endometrial tissue and restore normal pelvic anatomy. Surgical options include laparoscopy, a minimally invasive procedure. Studies have shown that surgical treatment can improve fertility rates, especially in women with severe endometriosis.
Assisted Reproductive Technology (ART)
In cases where medical and surgical treatments are unsuccessful, assisted reproductive technologies (ART) such as in vitro fertilization (IVF) may be considered. IVF involves the extraction of eggs from the ovaries, which are then fertilized with sperm in a laboratory. The resulting embryos are then transferred back into the uterus.
The Hope for Women with Endometriosis and Infertility
Despite the challenges posed by endometriosis, it’s crucial for women to know that having this condition does not necessarily mean they cannot get pregnant. With the right treatment approach, many women with endometriosis can successfully conceive and carry a pregnancy to term.
In conclusion, understanding how common infertility is with endometriosis is essential for providing effective treatment and support to women dealing with this condition. While endometriosis can indeed impact fertility, it’s important to remember that it’s not the end of the road. With advances in medical technology and treatments, many women with endometriosis are able to overcome their fertility challenges and fulfill their dreams of motherhood.
Read More: Life After Endometriosis Surgery: A Comprehensive Guide
References:
https://www.pennmedicine.org/updates/blogs/fertility-blog/2016/august/endometriosis-and-fertility
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3538128/
https://www.frontiersin.org/articles/10.3389/fsurg.2014.00024
https://obgyn.onlinelibrary.wiley.com/doi/10.1111/aogs.13082

Endometriosis-Related Infertility – Minimal Causes
Endometriosis, a common gynecological condition, has been frequently associated with infertility. However, the question remains: can minimal endometriosis cause infertility? This comprehensive article aims to delve into the connection between endometriosis, particularly in its minimal stage, and fertility issues.
Defining Endometriosis
Endometriosis is a medical condition characterized by the growth of endometrium-like tissues outside the uterus. These tissues can adhere to various pelvic structures like the ovaries, fallopian tubes, and even the intestines and bladder, causing irritation, inflammation, and scar tissue formation.
Stages of Endometriosis
Endometriosis is categorized into four stages:
- Stage I (Minimal): Small endometriotic implants with no scar tissue.
- Stage II (Mild): More extensive implants, involving less than 2 inches of the abdomen, without scar tissue.
- Stage III (Moderate): Severe endometriosis with deep implants and possible formation of endometriotic cysts or ‘chocolate cysts’ in the ovaries.
- Stage IV (Severe): Numerous endometriotic implants, possibly large endometriotic cysts in the ovaries, and scar tissue formation around the reproductive organs.
Read More: Understanding How Endometriosis Can Cause
The Connection Between Endometriosis and Infertility
It’s estimated that 30% to 50% of women with endometriosis may experience infertility. Even in cases of minimal or mild endometriosis, the disease may still impact fertility in numerous ways, including:
- Distorted pelvic anatomy due to scar tissue and adhesions
- Inflammatory response causing a hostile environment for eggs, sperm, and embryos
- Altered immune system functionality
- Changes in the hormonal environment affecting egg quality and embryo implantation
However, it’s essential to note that endometriosis does not necessarily equate to infertility. Many women with endometriosis, even in severe stages, can conceive naturally or with fertility treatments.
Exploring the Question: Can Minimal Endometriosis Cause Infertility?
The impact of minimal endometriosis on fertility is a contentious subject. The disease, even at its earliest stage, can cause inflammation and subtle changes in the pelvic environment, potentially affecting fertility. However, many women with minimal endometriosis conceive without issues, leading some researchers to suspect that other factors, possibly genetic or immunological, might be at play in cases of endometriosis-associated infertility.
Diagnosing Endometriosis
Diagnosing endometriosis can be challenging, as many women with infertility migh experience no symptoms. The gold standard for diagnosis is a surgical procedure known as laparoscopy, allowing the doctor to visually inspect the pelvic organs for endometriotic lesions and scar tissue, and take samples for histopathology.
Read More: Life After Endometriosis Surgery: A Comprehensive Guide
Evaluating Fertility
Before initiating any fertility treatment, a comprehensive fertility evaluation is recommended. This includes hormonal and blood tests, an assessment of ovarian reserve, a sperm analysis for the male partner, and possibly a laparoscopy to confirm the presence and extent of endometriosis.
Read More: Pelvic Floor Physical Therapy: What you Need to Know
Treatment Options for Endometriosis-Related Infertility
The treatment approach for endometriosis-related infertility is multifaceted, depending on the stage of endometriosis, the woman’s age, and the presence of other fertility factors.
Surgical Treatment
For women with Stage I or II endometriosis, surgical removal of endometriotic tissue may improve pregnancy rates. However, for women aged 35 or older, other fertility treatments might be recommended in addition to surgery.
Medical Treatment
Medical treatments aim to suppress endometriosis growth by reducing estrogen levels. However, these treatments, including hormonal contraceptives and Gonadotropin-Releasing Hormone (GnRH) agonists, prevent pregnancy during use.
Assisted Reproductive Technology (ART)
In cases where pregnancy does not occur naturally or following surgery, ART methods such as Intrauterine Insemination (IUI) or In Vitro Fertilization (IVF) may be recommended. The success rates of these treatments vary depending on the woman’s age, ovarian reserve, and specific fertility issues.
Conclusion: Can Minimal Endometriosis Cause Infertility?
While minimal endometriosis can potentially affect fertility, it does not guarantee infertility. A comprehensive evaluation and personalized treatment plan can help women with endometriosis, even at minimal stages, to conceive successfully. However, further research is needed to fully understand the complex relationship between endometriosis and fertility.
References:
https://www.uptodate.com/contents/endometriosis-treatment-of-infertility-in-females
Anti-Mullerian Hormone & Endometriosis – What’s The Connection?
Endometriosis has been associated with a marker called Antimullerian hormone (AMH), which is a pivotal marker of ovarian reserve, and is commonly measured in women with endometriosis specifically in relation to fertility. There is debate among the community that your AMH level is what it is and it cannot change. I would challenge this notion though as I have seen people with endometriosis have significant increases after proper excision surgery, which is a point of debate. Recently, I had another patient send me lab work that demonstrated what some may call a low AMH, has confirmed endometriosis, but likely a surgery that was incomplete and is continuing to suffer ongoing symptoms. Though I have seen this change in my patients, I recognize this is only a small fraction of the people suffering, so it was time to review what the research says. This article aims to provide a review of the various studies conducted on this critical subject, exploring how endometriosis and AMH interact, the effect of surgical intervention on AMH levels, and the subsequent impact on fertility.
The Antimullerian Hormone (AMH): A Brief Overview
AMH, a hormone playing diverse roles during embryonic development and puberty, is produced by ovarian follicles smaller than 8 mm, hence linking ovarian reserve to AMH levels in the blood. The normal range for AMH hovers between 1 and 4 ng/mL. However, women’s AMH levels greatly vary based on factors like age, ethnic background, lifestyle, and genetics. Additionally, someone at the low end of range may still suffer problems despite them being “in range.”
AMH Testing in Reproductive Health
AMH testing is a crucial tool for evaluating female fertility. It can assist in:
- Assisting with understanding the prognosis of a woman’s response to assisted reproduction techniques (ART) such as in vitro fertilization (IVF)
- Confirming other markers of menopause
- Providing a more comprehensive evaluation when certain conditions are confirmed or suspected such as polycystic ovarian syndrome (PCOS), premature ovarian failure, and endometriosis
Endometriosis and AMH Levels
Endometriosis is a common culprit behind infertility, affecting nearly half of the women suffering from this ailment. This infertility arises from various factors, including inflammation in the reproductive tract, scar tissue-induced decreased blood supply to the ovaries, and pelvic anatomical distortions. Research reveals a significant correlation between endometriosis and lower than average AMH levels.
Some argue that surgical intervention of endometriosis often leads to a reduction in AMH levels, though many of us in the community may argue that this is a more nuanced topic and this highly depends on the skill of the surgeon, something that is often overlooked in endometriosis research. Various studies have attempted to decipher the impact of endometriosis surgery on AMH levels and fertility outcomes. A retrospective study conducted in 2016 found that preoperative AMH levels did not influence pregnancy rates after surgery. This is consistent with the literature we have on surgical impact, and thus the need for better research in the future. In my experience, this is the opposite of what I have seen, as many of us have seen when people get to the right surgeon.
Laparoscopic Cystectomy on AMH Levels
Laparoscopic ovarian cystectomy, a common surgical procedure to treat endometriomas, has been associated with decreased ovarian reserve. A study in 2019 demonstrated significantly lower AMH levels in women who underwent laparoscopic endometrioma cystectomy, especially in cases with bilateral cysts larger than 7 cm and stage 4 endometriosis.
Considerations: I want to highlight that we do not know the skill of the surgeon, but we do know that the skill of the surgeon matters. That being said, large endometriomas can often overtake ovarian tissue which is what happened to Christina. Hear her story here. This is why it is extremely important to find a knowledgeable surgeon that you feel comfortable with. If you need help finding a surgeon, you can start here.
Laparoscopic Endometriosis Surgery on AMH Levels
A literature review and meta-analysis of 19 studies conducted between 2010 and 2019 on the impact of laparoscopic endometriosis surgery on AMH levels post-surgery revealed a decline in AMH levels, extending beyond six months post-surgery. This decline was more pronounced in cases where surgery was performed on both sides of the body, compared to a single side.
Again, I would argue that we consider the quality of the research and the skill of the surgeon. Remember, ablation is different from excision and this may be another factor that is skewing results. I repeat this because, like many of us in the community, this is not our experience, thus I often read research with these things in mind. If many others in the community are also seeing this, there must be more to consider than what is presented. The bottom line is that we need better research.
AMH Levels Post-Surgery for Endometrioma
Several studies have observed that laparoscopic ovarian cystectomy results in a significant and progressive decrease in AMH levels post-surgery. However, other studies have noted that this decrease may only be temporary, with levels potentially returning to normal within a year. Another factor to consider is when the AMH was measured post-surgery and what other factors may have impacted the levels!
Certain studies have observed a temporary decrease in AMH levels following endometrioma ablation. However, this decrease did not persist beyond six months in most cases, suggesting a potential recovery of ovarian reserves.
Several studies have compared the decrease in AMH levels following ovarian cystectomy and endometrioma vaporization. The general consensus suggests a higher postoperative decline in AMH levels following cystectomy compared to vaporization, particularly in bilateral endometrioma cases.
This caught my attention and highlights my thoughts on how the surgery (excision) is being performed as to not compromise ovarian tissue. Using ablation, which is what the CO2 laser is referring to, may not compromise the ovarian tissue, but it also may not treat the disease. Paul Tyan, MD discusses this complex topic in our interview which you can find here.
The combined technique, involving partial cystectomy and ablation, has been shown to have less detrimental effects on the ovary, resulting in a lesser decline in AMH levels post-surgery.
The role of endometriosis surgery in improving pregnancy rates remains a topic of debate. Some studies suggest that surgery might improve the success rates of fertility treatment, while others highlight the risk of ovarian damage due to surgical intervention.
In conclusion, the Antimullerian hormone is a vital marker for assessing the impact of endometriosis and its surgical intervention on ovarian reserve and fertility. Understanding the complex relationship between AMH levels, endometriosis, and surgical intervention along with identifying gaps in the research can help medical professionals devise more effective treatment strategies, improve the quality of research studies which ultimately improves patient outcomes.
IRelated Reading:
- Does Endometriosis Cause Infertility? Covering the Basics
- Endometriosis and Pregnancy: Natural, Medical, & Surgical Options
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6603105/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7865255/
- https://drseckin.com/endometriosis-surgery-and-amh-levels/

Can endometriosis cause miscarriage? Understanding Endometriosis and Its Impact on Miscarriage
Endometriosis is a prevalent health condition, affecting approximately 10% of women worldwide. It is often associated with chronic pain and infertility, but its potential connection to miscarriage is not as widely recognized. This article aims to shed light on the link between endometriosis and miscarriage, drawing on recent scientific research and expert insights.
What is Endometriosis?
Endometriosis is a chronic condition where tissue similar to the lining of the uterus, known as endometrium, grows outside the uterus. This tissue can grow on the ovaries, fallopian tubes, or the lining of the pelvic cavity. Just as the inner lining of the uterus thickens, breaks down, and bleeds with each menstrual cycle, so too does the endometrial-like tissue outside the uterus. However, this displaced tissue has no way to exit the body, leading to various problems.
Read More: What causes endometriosis?
Pathogenesis of Endometriosis
Endometriosis develops in stages, with severity ranging from minimal to severe. The American Society for Reproductive Medicine groups endometriosis into four stages: minimal (Stage I), mild (Stage II), moderate (Stage III), and severe (Stage IV). The stages reflect the extent, location, and depth of endometrial-like tissue growth, as well as the presence and severity of adhesions and the presence and size of ovarian endometriomas.
Symptoms of Endometriosis
While some women with endometriosis may have no symptoms, others may experience:
- Painful periods
- Pain during intercourse
- Pain with bowel movements or urination
- Excessive bleeding
- Infertility
- Other signs and symptoms such as fatigue, diarrhea, constipation, bloating, or nausea
Read more: 20 Signs and Symptoms of Endometriosis
Endometriosis and Pregnancy Complications
Endometriosis has long been associated with infertility, with studies indicating that up to 50% of women with infertility have the condition. However, less is known about its impact on women who do conceive. Emerging research suggests that endometriosis may increase the risk of several pregnancy complications, including preterm birth, cesarean delivery, and miscarriage.
Read More: How Does Endometriosis Cause Infertility?
Endometriosis and Miscarriage: Understanding the Connection
Recent research has begun to explore the potential link between endometriosis and miscarriage. Miscarriage, also known as spontaneous abortion, is defined as the loss of a pregnancy before 20 weeks of gestation. It is estimated that about 10-20% of known pregnancies end in miscarriage. The actual number is likely higher, as many miscarriages happen so early in pregnancy that a woman might not even know she’s pregnant.
The Role of Inflammation
One theory proposes that the inflammation associated with endometriosis could interfere with the early stages of pregnancy. Endometriosis is characterized by chronic pelvic inflammation, which could potentially disrupt the implantation of the embryo or the development of the placenta.
The Impact of Surgical Treatment
Another factor to consider is the potential impact of surgical treatment for endometriosis. There have only been a few clinical trials and they do not indicate that surgical excision reduces the risk of miscarriage. However, there are two very large databases from Sweden and Scotland that suggest a benefit to removing known endometriosis to lower pregnancy loss risk. More research is required.
Hormonal Factors
Endometriosis can alter the hormonal environment of the uterus, which could potentially impact early pregnancy. More research is needed to fully understand how these hormonal changes might contribute to miscarriage risk.
Research Insights: Endometriosis and Miscarriage Risk
Several studies have investigated the link between endometriosis and miscarriage. A meta-analysis published in 2020 in the journal BioMed Research International found that women with endometriosis had a significantly higher risk of miscarriage compared to women without the condition. This risk was particularly pronounced in women who conceived naturally, rather than those with tubal infertility who conceived through assisted reproductive technology (ART).
Coping with Endometriosis and Miscarriage
The potential link between endometriosis and miscarriage can come as distressing news. However, it’s important to remember that many women with endometriosis have successful pregnancies. So, counseling and intervention really depend on the individual situation. With repeat losses, there are many potential reasons but it appears that endo can be one of them.
Read more: Find an Endometriosis Specialist for Diagnosis, Treatment, & Surgery.
Conclusion
Endometriosis is a complex condition that can impact various aspects of a woman’s health, including her fertility and pregnancy outcomes. While research suggests a potential link between endometriosis and miscarriage, many women with the condition have successful pregnancies. If you have endometriosis or suspect you have endo, and having difficulty conceiving or experiencing pregnancy losses, it’s crucial to seek consultation with an endometriosis specialist.
Reference:
https://pubmed.ncbi.nlm.nih.gov/33490243/

How Does Endometriosis Cause Infertility?
Endometriosis, a complex and often misunderstood condition, can significantly impact a woman’s fertility. Understanding the intricacies of this condition, its causes, and its effects on fertility can be vital in paving the way for effective treatment strategies.
An Introduction to Endometriosis
Endometriosis is a benign, estrogen-dependent disorder primarily affecting approximately one in ten cisgender women in their reproductive years. It may also have an impact on transgender men, where the condition may be present in a higher percentage. While it has been reported in cisgender men, it is exceedingly rare. Thus the fertility impact discussed here is that which specifically affects the uterus, Fallopian tubes and ovaries.
Endometriosis is characterized by the abnormal presence of endometrial-like tissue outside the uterus. This abnormally growing tissue is often found in the pelvic region, such as on the ovaries, fallopian tubes, and the outer surface of the uterus. Still, in some cases, it can extend beyond the pelvic area.
While endometriosis affects approximately 10-15% of cisgender women in their reproductive years, the condition is more prevalent in those struggling with infertility, affecting up to 25%-50% of this demographic. The exact cause of endometriosis remains a subject of research and debate, and its impact on fertility is multi-faceted and complex.
Understanding The Pathogenesis of Endometriosis
While the precise cause of endometriosis is still under debate, several theories have emerged over the years, trying to explain the pathogenesis of this condition.
Retrograde Menstruation
The oldest theory is retrograde menstruation, which suggests that during menstruation, some of the endometrial tissue flows backward, through the fallopian tubes, into the pelvic cavity instead of leaving the body. These endometrial cells then attach to the peritoneal surfaces, proliferate, and form endometriosis implants.
Coelomic Metaplasia and Metastatic Spread
Other theories suggest that cells in the peritoneum can transform into endometrial cells, a process known as coelomic metaplasia. Alternatively, endometrial tissue may spread through the bloodstream or lymphatic system to other parts of the body, a process known as metastatic spread. Both these theories could explain how endometriosis implants can be found in areas outside the pelvic region.
Altered Immunity
Another theory proposes that women with endometriosis have a compromised immune system, which fails to eliminate the endometrial cells that have migrated to the peritoneal cavity. This immune dysfunction may also contribute to the progression of the disease, as the immune system’s reactions may inadvertently promote the growth and proliferation of endometrial implants.
Stem Cells and Genetics
Recent research also suggests that stem cells and genetic factors may play a role in the development of endometriosis. Bone marrow-derived stem cells may differentiate into endometriosis cells, contributing to the formation of ectopic endometrial-like tissue.
Additionally, genetic predisposition may play a significant role in the development of endometriosis. People with a first-degree relative affected by the disease have a seven times higher risk of developing endometriosis.
Learn More: Current Knowledge on Endometriosis Etiology: A Systematic Review
How Does Endometriosis Cause Infertility?
Endometriosis can affect fertility through various mechanisms:
Effect on Gametes and Embryo
Endometriosis can impact the production and quality of oocytes (eggs), as well as sperm function and embryo health. The presence of endometriomas (cysts caused by endometriosis) and the inflammatory environment they create can negatively affect both oocyte production and ovulation.
Effect on Fallopian Tubes and Embryo Transport
Endometriosis can disrupt the fallopian tubes’ normal functioning and impact the embryo’s transport. The inflammation caused by endometriosis can impair tubal motility and cause abnormal uterine contractions, which can hinder the transportation of gametes (eggs and sperm) and embryos.
Effect on the Endometrium
Endometriosis can also impact the uterine lining or endometrium, which can lead to implantation failure. Research suggests that endometriosis can alter the gene expression in the endometrium, affecting its receptivity to implantation.
Read More: Learn More About the Connections Between Endometriosis and Infertility
Current Treatment Options for Endometriosis-Associated Infertility
The treatment of endometriosis-associated infertility is multi-faceted and can include expectant management, medical treatment, surgical treatment, and assisted reproductive technologies.
Expectant Management
While endometriosis significantly lowers fertility rates, some women with mild to moderate endometriosis can still conceive without any medical or surgical intervention. However, this approach may be more suitable for younger women with mild endometriosis and no other fertility issues.
Surgical Treatment
Surgery can be both diagnostic and therapeutic in the context of endometriosis. The goal of surgical treatment is to remove or reduce endometriosis implants and restore normal pelvic anatomy and reduce the inflammatory impact. This could potentially improve fertility, particularly in women with severe endometriosis.
Assisted Reproductive Technology
In vitro fertilization (IVF) is currently the most effective treatment for endometriosis-associated infertility. IVF can be particularly beneficial for women with severe endometriosis or those for whom other treatments have failed.
Medical Treatment
Medical treatment for endometriosis primarily targets reducing the severity of the disease and relieving symptoms. Hormonal medications such as combined oral contraceptives, progestins, danazol, and gonadotropin-releasing hormone agonists or antagonists (GnRH analogs) are commonly used. However, these medications have not shown any significant benefit in treating endometriosis-associated infertility.
Read More: Natural, Medical & Surgical Treatment of Endometriosis Infertility
Looking Towards The Future: Potential Treatments
As our understanding of endometriosis deepens, new potential treatment options are emerging, such as therapies targeting the abnormal gene expression and inflammation caused by endometriosis. Furthermore, stem cell therapies and genetic interventions hold promise for treating endometriosis-associated infertility in the future. As research continues, the hope is that these advancements will lead to more effective strategies for managing this complex condition and improving fertility outcomes in those with endometriosis.
Read More: How Do Endo Fertility Issues Impact the Mental Health of a Person?
Reference: Macer ML, Taylor HS, Obstet Gynecol Clin North Am. 2012 Dec;39(4):535-49.

How Do Endo Fertility Issues Impact the Mental Health of a Person?
Endometriosis (endo) can cause many issues. Endometriosis patients may have difficulty becoming pregnant or maintaining a full-term pregnancy. Up to 70% of women with endometriosis get pregnant without medical treatment. However, 30 to 50% of patients with endo experience fertility issues and may need endometriosis fertility treatments or surgery. Up to 50% of all women with infertility have endometriosis. According to the abstract in a study published in the International Journal of Women’s Health:
“The most common clinical signs of endometriosis are menstrual irregularities, chronic pelvic pain (CPP), dysmenorrhea, dyspareunia and infertility. Symptoms of endometriosis often affect psychological and social functioning of patients. For this reason, endometriosis is considered as a disabling condition that may significantly compromise social relationships, sexuality and mental health.”
Why Are Women Impacted Emotionally By Reproductive Disorders?
A plethora of reasons exists as to why women can experience deep emotional impact by a diagnosis of a reproductive disorder or a condition that could cause issues with fertility. Some women already worry about getting pregnant anyway, so an endometriosis diagnosis surely doesn’t help. Here’s a shortlist of some reasons reproductive issues can affect the emotional health of women with endometriosis:
- Pressure to conceive right away
- Worries about each stage of the pregnancy, from implantation to delivery
- Pressured to have a child, even if the person is unsure or not ready
- Possible medical interventions, such as IVF
- Stress and emotional drainage that can result from endometriosis fertility treatments
- Possible laparoscopy endometriosis surgery
Multiple studies demonstrate that a woman’s ability to conceive and bear a child plays a big part in her emotional health and self-esteem. While many women don’t want to have children, a large portion does. But, they might not be ready for a baby when they receive their endometriosis diagnosis. According to a study out of the Iranian Journal of Reproductive Medicine:
“While infertility is not a disease, it and its treatment can affect all aspects of people’s lives, which can cause various psychological-emotional disorders or consequences including turmoil, frustration, depression, anxiety, hopelessness, guilt, and feelings of worthlessness in life.”
Endometriosis Patients with Fertility Issues Need Emotional Support
Most endometriosis patients with fertility issues benefit by having a mental health provider as part of their multidisciplinary team.
Endometriosis impacts many facets of a person’s life. A recent study concluded that:
“Furthermore, there is an urgent need to develop and evaluate interventions for supporting women and partners living with this chronic and often debilitating condition.”
All Endometriosis Patients Could Benefit From Emotional Support
Many endometriosis patients with fertility issues express no desire to have children. Therefore, some women are unaffected by infertility that might arise from endo. However, it’s essential to keep these women in mind because their feelings matter, too. Perhaps some did not want to have kids now but were hoping to someday in the future? Or maybe they are just not with the right person to have children with them?
Whatever the case may be, it’s significant that healthcare providers do not overlook a patient’s emotional needs, even if they say it doesn’t bother them if they cannot have kids. Perhaps a person in this situation may not need as intense emotional support, but they should see a mental health provider have a chance to talk about these feelings and think them through. Some interventions can help one conceive or be ready to conceive even with an endometriosis diagnosis. However, it’s significant to remember that the further the disease has progressed, the more complex it is to treat it to regain fertility. Therefore, when you are unsure if you want to have a baby, it’s still wise to have all the lesions removed as soon as you can and conduct proper follow-up.
Seeking a Mental Health Provider Experienced With Endometriosis
Endometriosis is a complex and often misunderstood disease. Therefore, women who battle this condition daily, especially those with fertility issues, require a mental health professional familiar with this inflammatory disorder.
Endometriosis encompasses many domains of a patient’s life, and fertility issues are not the only things that impact women’s emotional health. When seeking out a professional, it’s critical to find someone familiar with the disease and its emotional impact on patients.
Importance of Friends and Family
In addition to adding a robust mental health provider to your team, it’s also essential that you seek support from your loved ones. Please encourage them to attend appointments with you to have a better understanding of the condition. When the people closest to you can comprehend the emotional roller-coaster accompanying infertility, they will be better prepared to support you emotionally.
When a patient receives a diagnosis such as endometriosis, pain management, and other care items often become the priority. Therefore, it can be easy to overlook the emotional aspect of this condition, especially in someone with fertility issues. This is why it’s essential to do your research and find an experienced endometriosis expert to head up your team.
Do You Have Fertility Issues Caused By Endometriosis?
We want to hear from you. What are your thoughts on the emotional challenges? Do you have a solid mental health provider on your team? Leave your responses in the comments below.

Endometriosis Fertility Treatment: Natural, Medical, & Surgical Options
Natural, Medical & Surgical Treatment of Endometriosis Infertility
Endometriosis (endo) is a common condition that affects up to 10% of all women globally. But most people do not realize this condition’s impact on a significant proportion of women. Endometriosis and pregnancy complications are a common coincidence. Up to 50% of women with infertility have endo.
Endometriosis and pregnancy can be problematic for patients. And sometimes, endometriosis treatments are needed to conceive. Keep reading to learn more about fertility options for women with endo.
Read More: How Does Endometriosis Cause Infertility?
Lack of Evidence-Based Research Stalls Treatment Options
Endometriosis is sometimes like the elephant in the room that no one wants to discuss or do enough research. However, that needs to change because endometriosis is often a disabling condition, and people should know about it. Not only does this condition impact the patient’s quality of life, but it also affects the potential for some of these patients to have a family. This situation can affect a marriage, other family members, a partner, etc.
Options for treating women with endometriosis and pregnancy issues can be natural, medical, surgical, or surgery-assisted. Let’s review the latest fertility treatments and courses of action for women affected by endometriosis. First, we will briefly discuss how endometriosis and pregnancy are related.
Can You Get Pregnant with Endometriosis?
Natural
Getting pregnant with endometriosis is not always easy, but it’s a reality for most patients who have the condition and want to conceive. It’s important to emphasize that the body can and still does get pregnant. There are things such as an endometriosis diet that might help. Let’s look at the good numbers. Up to 70%, according to some studies, of women with mild to moderate endometriosis will become pregnant without medical intervention.
Medically-Assisted
Statistics show that about 75% of women with severe endometriosis (stage III/IV) will conceive if they desire. Two-thirds of those pregnancies occurred naturally, and one-third with the help of the endometriosis fertility treatment.
If you have endometriosis and are having troubles getting or maintaining a pregnancy, and you wish to carry full-term, here are some medical options that may interest you:
- Freeze some eggs: Your ovarian reserve of eggs can decline due to endometriosis. Therefore, some endo specialists recommend preserving your eggs in case you wish to conceive later. Just note that this can be an expensive option.
- Superovulation and intrauterine insemination (SO-IUI): If you have normal fallopian tubes, mild endometriosis, and a partner with healthy sperm, this might be the best choice for you.
- Fertility medications: Doctors can prescribe medications to produce up to two or three mature eggs. There are also progestin injections that are often used to help fertility issues.
- Frequent ultrasounds: If a person is trying to get pregnant, they may go in for frequent ultrasounds to identify when the eggs are most mature. At that time, a doctor can insert the partner’s collected sperm.
- In-Vitro Fertilization (IVF): This treatment involves the extraction of the egg and sperm. The egg is fertilized outside the body and then implanted into the uterus.
Endometriosis Surgery For Infertility
Many women with endometriosis do become pregnant without medical assistance. However, studies suggest that endometriosis surgery does help a woman to become pregnant without difficulty.
- Removal of endometriosis tissue: Evidence shows that pregnancy rates improve if the endometriosis tissues are removed surgically.
- Removal of tissue or large endometriosis cysts: Large cysts and tissue accumulation can contribute to infertility. Removing these can help the patient conceive.
- Routine follow-up: Women with endometriosis often have cysts that relapse after treatment. It is crucial to complete follow-up visits and possibly have complementary surgeries down the road.
How Your Stage of Endometriosis Impacts Fertility
A diagnosis of endometriosis is a heavy thing to take in, primarily since it’s known to impact a woman’s reproductive organs. Studies have shown that the extent of endometriosis present during laparoscopy correlates with fertility.
Do You Have Concerns About Endometriosis and Fertility?
We want to hear from you. What is your biggest concern about the fertility impact of endometriosis? Or does it concern you at all? Leave your answers in the comments below. If you need medical attention that is not emergent, be sure to find a vetted endometriosis specialist who is familiar with the disease and modern treatments.

Endometriosis and Fertility: Statistics, Facts, & Fiction
Debunking the Myths Surrounding Endometriosis and Reproduction
Disinformation about endometriosis and how it can impact reproduction is thick. As a matter of fact, not just endometriosis and fertility, the entire disorder is shrouded in junk information, and so it often goes misunderstood and mistreated. To learn more on this topic, read our previous article, titled: “Endometriosis Facts and Myths: Dispelling the Misconceptions.”
Does endometriosis cause infertility? In some cases, yes. However, in most cases, women with endometriosis can and do get pregnant without any medical assistance or intervention of any kind. There is still a myth that if you become pregnant, that can manage the endometriosis (endo) symptoms and even help resolve disease progression.
This statement couldn’t be further from the truth, and it’s an example of a widespread myth about endometriosis and fertility. Furthermore, this school of thought can put additional pressure on women with endometriosis to get pregnant as quickly as possible once they get a diagnosis. As you can imagine, this dangerous misinformation can alter their expectations in terms of treatment for fertility and their outlook on endometriosis in general.
So, Can You Get Pregnant If You Have Endometriosis?
The real truth is that the connection between endometriosis and reproduction is complex. Can you get pregnant if you have endometriosis? Yes, many people can and do. However, having the right endometriosis specialist to help you along the way can make all the difference in your journey. Click here to learn more about finding vetted endo specialists near you. In this article, we will review the disease and lay out the facts regarding endometriosis and fertility.
What is Endometriosis?
Endometriosis is an inflammatory disorder in which tissue similar to the uterus lining grows in places outside the uterus. Often these growths happen on the surface of the uterus, ovaries, fallopian tubes, or other organs within the pelvic cavity – such as the bladder or bowel. In some cases, these endometriosis growths have occurred in distant organs.
Endo growths can cause pain, scarring, and sometimes infertility. Because this tissue is similar to the uterine lining, it also bleeds and sheds once a month during hormonal changes. Typically in the uterus, this period tissue and blood have a means of escaping through the vagina. However, this blood and tissue often accumulate inside the body with endometriosis and causes inflammation and pain. As one can imagine, over time, scar tissue growths with subsequent menstrual cycles develop. Eventually, this scar tissue can fuse organs, immobilize organs, and even damage the fallopian tubes.
Alarming Statistics About Endometriosis & Fertility
- Endometriosis is widespread, affecting between six and ten percent of the general female population. That’s more than 170 million worldwide.
- In patients with pelvic pain, infertility, or both, endometriosis frequency is higher – between 35 percent to 50 percent.
- Between 25 percent to 50 percent of infertile women have endometriosis.
- Between 30 percent to 50 percent of women with endometriosis are infertile.
- Endometriosis affects approximately the same number of women around the world that have diabetes.
- The cost of endometriosis in the US is between $86 Bn – $116 Bn.
- It takes, on average, eight years from the onset of symptoms for a patient to get a diagnosis. This can impact all patients, but especially those of who wish to keep their fertility intact.
Endometriosis Facts About Fertility and Reproduction
- There are ways to get pregnant with endometriosis.
- Hormonal therapy does not cure endo.
- Endometriosis is related to your menstrual cycle and hormonal changes within your body.
- Endometriosis tissue can be removed during laparoscopy. Depending on the location of the growths and the extent of damage, this can sometimes restore fertility.
- There is a type of endometriosis that can cause cancerous lesions, typically dark chocolate brown.
- The causes are uncertain, and there is no “cure” for endometriosis.
- Genes seem to play a role in the occurrence of endo.
Myths About Endometriosis and Fertility
- Pregnancy is not a cure or a way to relieve symptoms of endometriosis. Women should not be pressured or encouraged to get pregnant to help with endometriosis and fertility or alleviate pain or other symptoms. While some women experience less endo pain and symptoms during their period, that does not mean it works the same for all women.
- Do not believe any physician that tells you a hysterectomy is the “gold standard” treatment for endometriosis. As mentioned above, there is no “cure” for endometriosis. Until a specialist is inside the body and can view the number and the placement of the endometriosis lesions, they cannot decide whether a hysterectomy would even solve the problems. Also, some women might make themselves infertile (whether they mind or not, it is an emotional part of this disorder) by having a hysterectomy done that was never needed.
- You do not need to have a major medical procedure to get an endometriosis diagnosis or remove some growths and lesions. With modern equipment, skilled specialists, and advanced technology (often robotic surgical equipment), you can have endometriosis diagnosis and treatment with laparoscopy. This type of procedure is minimally invasive and only leaves behind a few puncture wounds.
- Abortion does not cause endometriosis.
- Endometriosis does not cause ovarian cancer. Although a type of endo involves cancerous tumors, this does not mean that having endometriosis makes you more likely to develop cancer.
- The most important myth to bust is that there is no treatment for endometriosis. Just because there is no “cure” for this pelvic inflammatory disorder does not mean there are no treatment options, even when it comes to endometriosis and infertility.
If you have endometriosis, what is the most common thing you have heard regarding endo and reproduction?

Does Endometriosis Cause Infertility? Covering the Basics
Learn More About the Connections Between Endometriosis and Infertility
An endometriosis (endo) diagnosis can be a frightening thing. Very frightening. While this inflammatory condition can be binary or non-binary, women of childbearing age are prone to issues with reproduction due to endo. So does endometriosis cause infertility? Keep reading as I break down the basics of this topic. In this comprehensive guide, I will delve into the complex interplay between endometriosis and fertility, exploring the condition’s impact, treatment options, and strategies to overcome potential obstacles on the journey to parenthood. I will also discuss the emotional impact of this condition on patients.
What is Endometriosis?
Endometriosis is a chronic inflammatory condition. In this disease, endometrial-like lesions implant on tissues and organs throughout the abdomen and pelvis, even elsewhere in the body! These lesions contain glands and stroma, similar to the endometrium (the tissue that lines the uterine walls), causing chronic inflammatory reactions.
Endometriosis lesions produce many substances and even make their own estrogen, which, as a result, causes a variety of issues locally and systemically. Pain is one of the most common symptoms, though silent endo exists as well. Please continue reading this article to learn more about endometriosis.
Endometriosis and Fertility: Exploring the Connection
While endometriosis does not automatically equate to infertility, there is a well-documented association between the two. Approximately 30% to 50% of individuals with endometriosis experience fertility challenges, though the reasons behind this link are not fully understood. Several potential mechanisms have been proposed:
- Anatomical Distortions: Endometriosis can cause physical distortions in the reproductive anatomy, leading to scarring, adhesions, and obstructions in the fallopian tubes or ovaries, hindering the fertilization process.
- Inflammatory Response: The lesions can trigger an inflammatory response, creating an inhospitable environment for fertilization and implantation.
- Hormonal Imbalances: Endometriosis may disrupt the delicate hormonal balance required for ovulation and implantation, potentially impacting fertility.
- Egg Quality: Some research suggests that endometriosis may adversely affect egg quality, further complicating the conception process.
Despite these potential challenges, it’s important to note that more than 70% of individuals with mild to moderate endometriosis can conceive naturally, offering hope for those seeking to start a family.
What Happens When Endometriosis Does Cause Infertility?
It can. 25 to 50% of women with infertility have endometriosis, and 30 to 50% of women with endometriosis have infertility. However, it is very encouraging to know that most women with endometriosis can become pregnant.
This statistic is significant. Many younger women with this disorder feel psychological effects due to the possibility of not being able to have kids. Not all patients carry this sentiment. Growing numbers of people do not want to have children. However, for those who do, these thoughts and emotions about fertility can be devastating. Then, endometriosis patients who do conceive often worry about the pregnancy and subsequent delivery of the baby.
Other Data on Endometriosis and Reproduction
Studies have also demonstrated that the enzyme aromatase may also play a role in endometriosis and infertility. There is an abnormally high level of this enzyme in the endometrium and endometriosis lesions in patients with endometriosis. In the uterus, this enzyme may affect both natural endometrial development and its receptivity for the implantation of the fetus.
Progesterone is another hormone that may play a role in implantation failure. Resistance to this enzyme can affect reproduction, as it is necessary for a normal pregnancy. In some studies, progesterone receptors displayed abnormalities and caused dysregulation in the endometrial layer of the uterus in patients with endometriosis. Levels of progesterone should increase with pregnancy, but with endometriosis, this process is delayed and can cause an unopposed estrogen state that cannot sustain fertility.
Diagnosing Endometriosis: A Multifaceted Approach
Diagnosing endometriosis can be a complex process, as the symptoms can mimic those of other conditions. The diagnostic journey often begins with a physical examination and an evaluation of the individual’s medical history. If endometriosis is suspected, additional tests may be recommended, such as:
- Ultrasound: An abdominal or transvaginal ultrasound can help identify cysts (endometriomas), possibly endometriosis lesions (this is not common but an up-and-coming area of research), as well as the potential impact on the organs themselves or other abnormalities in the reproductive organs.
- Laparoscopy: Considered the gold standard for diagnosing endometriosis, a laparoscopy involves a minimally invasive surgical procedure where a small camera is inserted into the abdomen, allowing the surgeon to visually inspect the pelvic organs and take tissue samples if necessary.
While the severity of endometriosis is often classified into stages (minimal, mild, moderate, or severe) based on the extent and location of the endometrial growths, it’s important to note that the stage does not necessarily correlate with the intensity of symptoms or the degree of fertility challenges.
Managing Endometriosis: A Multidisciplinary Approach
The management of endometriosis typically involves a multidisciplinary approach, combining medical and surgical interventions tailored to the individual’s unique circumstances and fertility goals. Treatment options may include:
- Pain Management: Over-the-counter or prescription pain medications, such as non-steroidal anti-inflammatory drugs (NSAIDs) or hormonal contraceptives, can help alleviate the discomfort associated with endometriosis.
- Hormone Therapy: Hormonal treatments, such as birth control pills, progestin-only therapy, or gonadotropin-releasing hormone (GnRH) agonists, may have some impact on suppressing the growth of endometriosis and managing symptoms, though these options are only short-term while on the medications and can have some serious side effects.
- Surgery: Laparoscopic or robotic surgery is recommended to remove endometriosis, scar tissue, or cysts, potentially improving fertility outcomes.
- Assisted Reproductive Technologies (ART): In cases where natural conception remains challenging, assisted reproductive technologies like in vitro fertilization (IVF) or intrauterine insemination (IUI) may be recommended.
It’s crucial to work closely with a multidisciplinary team, including reproductive endocrinologists, gynecologists, and fertility specialists, to develop a personalized treatment plan that addresses both the management of endometriosis symptoms and the individual’s fertility goals.
Dietary and Lifestyle Considerations
While there is no definitive evidence that specific dietary or lifestyle changes can cure endometriosis or improve fertility outcomes, maintaining a healthy lifestyle can contribute to overall well-being and potentially alleviate some symptoms. Recommendations may include:
- Balanced Diet: Consuming a diet rich in fresh fruits, and vegetables, minimizing grains, especially gluten, and lean proteins can provide essential nutrients and support overall health.
- Exercise: Regular physical activity, such as low-impact exercises like walking or swimming, can help manage stress and promote overall well-being.
- Stress Management: Engaging in stress-reducing activities like meditation, yoga, or deep breathing exercises can help promote relaxation and reduce the impact of stress on fertility.
- Supplements: While the evidence is limited, some individuals report benefits from taking supplements for pain relief, reducing inflammation, and improving their quality of life.
It’s essential to consult with a healthcare professional before making significant dietary or lifestyle changes, especially if you are undergoing fertility treatments or considering assisted reproductive technologies.
Endometriosis and Pregnancy: Potential Complications
While endometriosis does not necessarily preclude a successful pregnancy, it’s important to be aware of potential complications that may arise. Some of the risks associated with endometriosis during pregnancy include:
- Placenta Previa: Endometriosis may increase the risk of placenta previa, a condition where the placenta partially or completely covers the cervix, potentially leading to bleeding and complications during pregnancy or delivery.
- Miscarriage: Research findings on the link between endometriosis and miscarriage have been mixed, with some studies suggesting an increased risk while others found no significant association.
- Ectopic Pregnancy: Endometriosis may increase the risk of ectopic pregnancy, where the fertilized egg implants outside the uterus, typically in the fallopian tube.
It’s essential to work closely with your healthcare provider to monitor and manage any potential complications that may arise during pregnancy if you have endometriosis.
Mental Well-Being and Psychological Impact of Fertility Treatment for Endo Patients
Living with endometriosis can be a challenging and emotionally taxing experience, particularly for those struggling with fertility issues. The physical pain, emotional distress, and potential financial burdens associated with treatment can take a toll on an individual’s mental well-being. It’s crucial to prioritize self-care and seek support from mental health professionals, support groups, or counseling services if needed.
Furthermore, you and your partner can do these things to help prepare for these possible feelings:
- Prepare and be ready for the emotional journey ahead.
- Cope with grief and loss associated with unsuccessful prior attempts or miscarriages.
- Develop strategies for coping with the news of other people’s births and pregnancies.
- Keep the communication lines between you and your partner open and discuss feelings throughout the entire process.
Endometriosis and Fertility: Navigating the Journey
The path to parenthood for individuals with endometriosis can be challenging, but it’s important to remember that fertility challenges are not insurmountable. By working closely with a multidisciplinary team of healthcare professionals, exploring various treatment options, and maintaining a positive outlook, many individuals with endometriosis can achieve their dream of starting a family.
It’s crucial to be proactive in seeking support and guidance from healthcare providers, as well as accessing resources and support networks specifically designed for those navigating endometriosis and fertility challenges. Organizations like the American Society for Reproductive Medicine (ASRM) and Endometriosis UK offer valuable information, resources, and advocacy support for individuals on this journey.
While endometriosis may present obstacles, embracing a comprehensive approach that addresses both the condition and fertility goals can increase the chances of a successful outcome. With perseverance, the right medical support, and a commitment to self-care, the dream of parenthood can become a reality for many individuals with endometriosis.
REFERENCES
https://www.pennmedicine.org/updates/blogs/fertility-blog/2016/august/endometriosis-and-fertility
https://www.endometriosis-uk.org/endometriosis-fertility-and-pregnanc
Updated: August 9, 2024

